Diane’s farewell message
After 52 years at WAMU, Diane Rehm says goodbye.
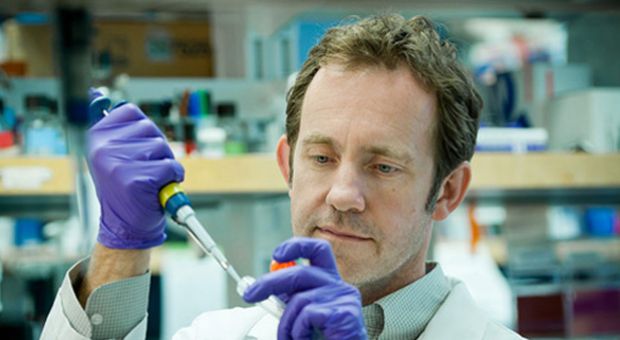
Matthew Farrer, appointed to the Dr. Donald Rix B.C. Leadership Chair in Genetic Medicine, works in his lab at the University of B.C. The Province’s Leading Edge Endowment Fund chair supports the world-class scientist’s work in identifying genes related to Parkinson’s, which is expected to lead to therapies that will arrest and prevent the disease.
Every year, 60,000 people in the U.S. are diagnosed with Parkinson’s disease. The devastating neurological disorder occurs when cells in the brain don’t produce enough dopamine. Most people know Parkinson’s for its physical symptoms: tremors, stiff muscles and slow movement. But the disease can also be marked by cognitive impairment and depression. And doctors now believe that Parkinson’s can cause changes to the brain years before it presents any physical symptoms. As public awareness increases, a discussion about the latest treatments for Parkinson’s, prospects for a cure, and the personal story of journalist Michael Kinsley.
MS. DIANE REHMThanks for joining us. I'm Diane Rehm. Parkinson's disease affects 1 million people in the U.S., nearly 10 million worldwide. Most people know it as a movement disorder that causes tremors and other physical symptoms, but doctors now believe the cognitive effects of the disease may occur years before diagnosis.
MS. DIANE REHMJoining me in the studio to talk about the latest research on Parkinson's disease: Dr. Walter Koroshetz of the National Institute for Neurological Disorders and Stroke, journalist and political commentator Michael Kinsley, and Dr. Zoltan Mari of Johns Hopkins University Medical School. Joining us by phone from New York, Dr. Mark Mapstone of the University of Rochester Medical Center. I hope you'll join the conversation. Give us a call at 800-433-8850. Send your email to drshow@wamu.org. Follow us on Facebook or send us a tweet. Thank you all for joining us.
MR. MICHAEL KINSLEYThank you, Diane.
DR. WALTER KOROSHETZPleasure here.
DR. ZOLTAN MARIThank you.
DR. MARK MAPSTONEThank you.
REHMGood to have you all here. Start with you, Dr. Koroshetz. Number one, I get the impression that the incidents of Parkinson's is going up. Am I incorrect about that?
KOROSHETZWell, Diane, as in most things, it depends on your definition. So I think what we've learned most recently is the biological nature of Parkinson's disease, and that probably does affect more people than we initially thought. So if you, you know, most people think of Parkinson's from the movie "Awakenings," where there's a problem with movement. Patients can't move, and they're frozen. A medicine was given, and, all of a sudden, they came back to life. And that is truth, that in the early stages of the disease, the medicines are incredibly effective at reducing symptoms.
REHMAs I understand it, it is a disease of the brain where the brain does not manufacture sufficient dopamine, correct?
KOROSHETZWell, I think that's part of it, but I think that's related to what we initially were saying about the effect of the medicines. But, in actual fact, now we know the biological basis of Parkinson's, and it is a neurodegenerative disease. And it's related, we think, to the deposition of aggregates of synuclein, a particular protein.
KOROSHETZAnd that actually occurs not just in the brain, but it may actually start in the nerves that are outside the brain that are going to the gut or to the nose or to the glands. The thought now is that this process, although it may begin outside, begins to move into the brain to the area of the brain stem where there are the cells that make dopamine.
KOROSHETZBut there are also other areas we call nuclei that make other transmitters, like acetylcholine or serotonin or adrenalin. These get affected early on, but this process doesn't stop there, unfortunately. It continues to move throughout the brain and affect cells in the circuit areas for our thinking, emotions, and really affects the ability of a person to be who they were.
REHMAnd so what are the most common outwardly visible signs of Parkinson's?
KOROSHETZWell, very good question, and this is a big question for the early signs. What we'd like to do is to be able to diagnose Parkinson's before it causes and enters the brain. People think that this may be -- the signature of this stage may be things like constipation, like a particular type of sleep disorder or restless leg syndrome. These are common conditions, but a certain percentage of people who have these go on to develop Parkinson's. And we think these are the early signs of this biological synuclein problem.
REHMAnd turning to you, Dr. Zoltan Mari, having heard this sort of what's going on in the brain, what do we know that causes Parkinson's?
MARISo we don't know a single cause for Parkinson's disease. It appears to be that there may be several different factors and causes together. Some of them relate to genetics, so very certainly certain kinds of genetic predispositions and genes that we know, that if you have a mutation, these genes, you have a higher likelihood of developing Parkinson's disease later in life.
MARIWe don't have a direct relationship with any one gene causing Parkinson's disease like we know for Huntington's disease. If you're genetically abnormal, it's just a question of time before you develop Huntington's disease. Whereas in Parkinson's disease, even if you have a mutation in one of these genes that are associated with Parkinson's disease, you only have an increased risk of developing. It's not a certainty.
REHMI see. Now, someone mentioned to me the other day that a diminished level of vitamin B12 may be a factor in someone's developing a movement disorder like Parkinson's later in life. Have you found that?
MARISo I've seen those reports, and many other vitamins and other environmental exposures have been associated with movement disorders and Parkinson's disease. To study these in a scientifically sound and statistically proper way is very hard. You have to do it prospectively 'cause looking at retrospective data, it could be a confound that you don't know that can affect your conclusions.
MARISo these are very important in discussing the causes of Parkinson's disease. I was going to move on the environmental exposures. Together with the genetic predisposition, many different kinds of environmental exposures could be relevant to the cause of Parkinson's disease, such as pesticides, drinking well water, others. Some of the currently used animal models of Parkinson's disease relate to some of these toxins that may occur in the environment.
REHMAnd turning to you, Michael Kinsley, you wrote a piece for last week's New Yorker titled "Have You Lost Your Mind?" And this is a personal history about your own life with Parkinson's disease. When were you actually first diagnosed?
KINSLEYWell, Diane, let me say first that my experience with Parkinson's cognitive problems so far has been purely theoretical, I'm glad to say. But I was diagnosed about 20 years ago.
REHMTwenty years ago, and what were the signs that you were experiencing?
KINSLEYWell, I went to my internist, and I said, my left hand -- I think it was my left. I can't even remember. Then my right -- one of my hands were a little stiff. And he said, hmm, you ought to see a neurologist. Then the neurologist said I probably had Parkinson's.
REHMSo you've been public about your disease now for many years, but at first, it took you a while to make full disclosure.
KINSLEYYes. I kept it secret as long as I could, which was about eight years.
REHMWhy?
KINSLEYWell, you don't want to walk around with people thinking you're sick if you don't have to. And my feeling was if -- I wrote a piece called "In Defense of Denial." And denial is a very effective strategy. You just don't think about it. But it only works if everyone else around you doesn't know.
REHMAnd were you experiencing a movement disorder in addition to your left or right hand?
KINSLEYWell, when -- I would say now my symptoms are less evident than they were when I first went to the doctor because I'm on medication. Obviously, if the medication were not available, I would be in much worse shape.
REHMAnd you also underwent deep brain stimulation. Now, how effective do you believe that actually was?
KINSLEYI believe, in my case at least, it was almost completely effective.
REHMAs far as the movement.
KINSLEYThe movement, yes. I have wires in my brain, and they go down to pacemakers essentially in my chest. And the pacemakers send little zaps into the brain, and they seem to work wonders.
REHMNow, do you believe that that deep brain stimulation affected you at all cognitively?
KINSLEYI didn't notice anything, but Mark Mapstone, I know, has done some research on that subject.
REHMAnd let's turn to Mark Mapstone. What's involved with the cognitive testing for Parkinson's, the likes of which you did on Michael Kinsley?
MAPSTONEWell, Diane, there's a number of different things that we do when we do cognitive assessments, much like the neurologists do when they do the motor assessments of the motor features of the disease. We're interested in specific cognitive features that, over years, we've learned through research and clinical practice are affected in the stages of the disease at different levels.
MAPSTONEAnd so at early diagnosis, we're interested in looking for very subtle things that are particularly useful for determining the accuracy of the diagnosis, just to make sure that this is Parkinson's disease and not some other disorder that can look a lot like Parkinson's.
REHMSuch as?
MAPSTONEWell, we've got things like Dementia with Lewy Bodies, multiple system atrophy, all sorts of different things that can appear like Parkinson's disease that come with different sorts or different flavors of cognitive symptoms. And so the early testing that we do is really designed to look at helping with initial diagnosis and making sure that this is Parkinson's. Bu that being said, there are some cases that do have -- of Parkinson's disease who do have some cognitive problems early on.
REHMDr. Mark Mapstone, he's a neuropsychologist and researcher in the field of cognitive neuroscience at the University of Rochester Medical Center. Short break here. We'll be right back.
REHMAnd just before the break we were talking with neuropsychologist Dr. Mark Mapstone about testing he does to determine, among other things, executive functioning on the part of people with various disorders. And you, Michael Kinsley, were tested back in the '90s. And what was found then?
KINSLEYWell, Mark could say better than me, but he tested me 20 years ago. And then I had some more tests before I had the operation you mentioned eight years ago. And both of those tests I passed with flying colors.
REHMOK.
KINSLEYAnd then I had some testing again, and there were some deficits, as they call them, but nothing that's, you know, I don't want anyone to be alarmed.
REHMDr. Mapstone, do you want to talk about that?
MAPSTONESure, sure. So the initial set of tests that we did at MIT in I believe it was 1994 were part of a research protocol. And Michael had volunteered very graciously to help with science after he was newly diagnosed, and we were doing research on trying to understand some of the early cognitive symptoms that we might find in patients with very detailed testing.
MAPSTONEAnd I might want to back up Michael's point that you really have to go looking for these deficits mostly in patients to find them. These are not evident things. And particularly when we tested him in the early '90s, found very little. As a matter of fact, he was off the charts on most of the things that I tested him.
MAPSTONEHe was doing very, very well, as to be expected. And I was quite impressed. In reviewing his data from about 2008 or so when he -- just before his surgery, again, he looked to be in very good shape. And the data looked very strong, particularly in the areas of executive function and memory and language.
REHMHelp me to understand what you mean by executive functioning.
MAPSTONESure, sure. So this is a term we use to describe a set of thinking abilities that people use to -- for higher order decision-making, planning, impulse control, the ability to do very complicated things that make us uniquely human. And although some lower species do have some of these abilities, we have them developed in very, very strong ways that allow us to do the things that we can do as human beings. And these are mostly things along the lines of decision-making and planning.
REHMAnd give me an example of a question you might ask.
MAPSTONEWell, for example, one might be to plan out in a series of steps, ways that you might operationally move from a stack of blocks, for example, from one area of the room to another area of the room. But there are certain rules. You can't put a big block on top of a small block. You can't put -- you can't make multiple moves at once. You have to do them one at a time. And if you make many errors -- you're trying to do this in as an efficient way as possible. If you make many errors, then that's an inefficient strategy, and you're really trying to be the most efficient as you can.
REHMSo after you tested Michael in 2008, just before he had the deep brain stimulation, then you tested him again more recently. And what did that indicate?
MAPSTONEWell, just to be clear first, I did not do the testing in 2008 before his surgery. That was at the Cleveland Clinic. And then the most recent set of tests were done at the University of Pennsylvania. So the last two sets I just had the data, but I did do the testing in the 1990s.
MAPSTONEAnd what we saw with the most recent set of tests was a little decline in some of these executive functions. And again, I have to emphasize that these are things that we can only pick up with these sensitive tests. These are probably not things that you're going to notice on a day-to-day basis with someone like Michael or at the state of Parkinson's that he has.
REHMAnd to you, Dr. Koroshetz, talk about deep brain stimulation, what it can and cannot do.
KOROSHETZWell, it's really quite an amazing feat that scientists studying monkeys, outline the circuits that are involved in control of motion. They were then able to use a toxin to cause a Parkinsonian-like symptom in the monkeys, found the abnormal circuits, and then found that they could put a wire into the brain, stimulate the deep parts of the brain, and the animal would all of a sudden lose all its deficits. And that also occurs in patients. It's one of the most amazing things to see.
KOROSHETZIt is basically trying to reset circuits that have been made abnormal by the pathology of Parkinson's disease. But these circuits are deep in the brain. They effect large parts of the brain like the frontal part where the executive function is really centered. The trouble with the deep brain stimulation is that it is a prude tool. We are injecting current to the brain. It's probably doing lots of things besides the ones we know about, besides the ones it was designated for. And it does not slow down the progression of the neurodegeneration. So it's more of a symptomatic therapy.
REHMAll right. And, Dr. Mari, the question becomes, are there less or noninvasive strategies being developed to treat the brain with that same outcome?
MARIYes. And I'd just like to emphasize that these are all symptomatic treatments including DBS, the medications. So far all the approved treatments available for Parkinson's disease are symptomatic. They don't actually change the underlying pathology in the progression. So we have to keep that in mind. And the Holy Grail remains finding this is modifying treatments that will actually change the underlying pathology.
MARIBut coming back to the noninvasive resetting of the networks, we have been involved with some research using transcranial direct current stimulation. So, as Dr. Koroshetz mentioned, this is a way to interfere with the network properties of the brain which is downstream from where the problem is, missing dopamine and other problems. And we are trying to intervene electrophysiologically to compensate for what went wrong.
REHMWithout going into the brain.
MARIWithout going into the brain. I have to say that this is experimental. It hasn't been fully proven as a treatment. And we are just trying to see if we can improve patients' motor functions through a method whereby we mount some electrodes outside of the brain, basically taping it onto the skin. And then pass some low electric current to the superficial parts of the brain. And that seems to be, if it's used right in certain circumstances, help make the motor functions better. And that would be a very interesting addition to our armamentarium of symptomatic treatment options.
KINSLEYBut you'd have to have your head shaved for the rest of your life.
MARIWell, we are looking at options whereby we could put the electrode underneath the skin which would still be less invasive than going through deep part of the brain.
REHMI see.
MARIAnd it's been known that transcranial magnetic stimulation produce some improvements in motor function before, but nobody can carry around a huge magnetic generator.
REHMOf course.
MARISo in terms of the practical applicability of such findings and therapy options, with all the current stimulation would be more interesting because you could carry a small battery with you. And, again, there are patients -- it's not a replacement for DBS. It never will be, but certainly it can delay the time to DBS. It can reduce the escalating needs of pharmacotherapy over the years of progression. Ideally, I mean, again, we are still looking at this, but it is very promising so far. And we are in the process of designing more experiments that go longer.
KINSLEYOne of the things they tell you after you have this operation is stay away from big refrigerators because they have magnets in them. And they can turn off your device without your realizing it.
REHMNow, do you carry that device with you, or is it implanted?
KINSLEYI've got two. Both are implanted on either side of my chest. And you have to look pretty carefully.
REHMYou have to look carefully in order to be able to see them.
KINSLEYYes.
REHMBut do they operate satisfactorily for you, or do they need adjustment?
KINSLEYYou have to -- when you first get it, you go for two or three appointments while they -- or more perhaps while they adjust it. And then the batteries do run out. So every four or five years, you have to get them replaced.
REHMI see. Dr. Mari, how typical a Parkinson's patient is Michael Kinsley?
MARIWell, I would say he's not typical in some ways, but at the same time, we do see, as we discussed in the last show, patients go 20 years, remain very highly functioning. I myself have several patients who are around 20 years into the disease and live alone, and they are fully functional. Most patients, however, 20 years into Parkinson's disease, will lose more ground than Michael.
MARIThey will be possibly cognitively more impaired. There are other non-motor problems including depression, anxiety, sleep issues, et cetera. And they are usually motor-wise progress a little more. But I have to say that 20 years out the majority of patients will report that their primary source of disability will be the non-motor issues other than the motor problems.
REHMNon-motor issues such as...
MARISuch as tremor. Tremor seems to be an early sign which draws attention. But at the same time, 20 years out, it is rarely any concern to anyone, slowing, but it can easy up, which is one of the most cardinal motor signs. These tend to respond very well to DBS and other symptomatic treatments. So generally treating motor symptoms we have tools. Even though we can't stop the progression of the disease, the symptomatic treatments are very effective, treating these motor symptoms. We are much less able to treat non-motor symptoms.
REHMSo using drugs, for example, to enhance dopamine in the brain helps considerably.
MARIExactly. So most of the pharmacotherapy centered on dopamine. We discussed in the beginning that early on Parkinson's disease was realized as a dopamine problem. And this was the dopamine-centric thinking and school of thought. More recently, we realize that dopamine is just one part of the picture. But dopamine deficit explains or relates to much of the motor problems.
MARISo if you do a dopamine-related pharmacotherapy, such as replacement or substitution of the missing dopamine or mimicking it with dopamine agonists tend to treat these motor symptoms quite well. And we have new therapies coming up in which the dopamine can be infused to the (word?) directly.
REHMInteresting. Dr. Zoltan Mari, he's at the Johns Hopkins University School of Medicine. And you're listening to "The Diane Rehm Show." Dr. Koroshetz, before we open the phones, is there a Parkinson's personality that shows itself prior to any symptoms that might appear?
KOROSHETZYou know, Diane, I don't think so. I think that Parkinson's can affect people of all personalities and subtypes. I don't think that's true.
REHMMichael, do you think so?
KINSLEYWell, I don't know. Some people say there is a Parkinsonian personality, including some neurologists. So, I mean, I guess you can legitimately disagree on that.
KOROSHETZOnce you have Parkinson's, then there are some changes, yeah.
REHMYeah. What about you, Dr. Mari?
MARII agree with Michael. I think there seems to be some tendency to it, but studying it is very hard because you don't necessarily have the right personality measurement tools to make a perspective study like that. But many clinicians agree that Parkinson's patients tend to be very nice people. They are usually very generous, et cetera. And of course it's not everyone, so just like with any other biological measure, there is always a spectrum and some distribution. There are patients of any kind. But there is some tendency nevertheless for the majority to fall in some personality trait in my opinion.
REHMSuch as...
MARINice, kind people, generous, unselfish. That's how...
REHMPunctual?
MARIPunctual, as detail oriented.
REHMRisk averse?
MARIPerhaps.
REHMDepressed?
MARINo. I don't think that they are -- have a greater rate of depression prior to their disease, although again we don't have a lot of perspective good data on this.
REHMDr. Mapstone, do you want to chime in?
MAPSTONEYeah, so I do see a little bit of this I think as anecdotally in my clinical practice where you do see characteristics that tend to show up in patients who have the early disease. And certainly, by the time they come to see us, they've had the disease. But what I think might be going on is really this might be a reflection of some of the early neurodegenerative changes that have been taking place possibly for years or even longer, prior to the onset of the defining motor symptoms of the disease.
MAPSTONEAnd so there might be things going on, as Dr. Koroshetz mentioned, about the preclinical symptoms like constipation, difficulty with smell and things like this, that might be going on way before the motor symptoms become bad enough to have them show up at the doctor's office for a diagnosis.
REHMMichael Kinsley, how good is or was your sense of smell?
KINSLEYWell, it's pretty bad, and that was one of the clues that went to my diagnosis.
REHMFairly widespread, Dr. Koroshetz.
KOROSHETZRight. I think this is -- I mean, this is really the exciting part of the science that we think that Parkinson's disease, the actual biology of the disease, is going on for 10 or 15 years before anyone knows they have it. So these personality traits, the trouble with smell, the trouble with constipation, the trouble with sleep, they are part of the disease.
KOROSHETZThe definition needs to change. The definition has to be based on the biological base of the disease. But what the beauty of this is that we think that now we can target -- if we can find these people, have a good therapy, we can target the disease 15 years before there's any symptoms. And potentially that's a cure. So that's, I think, what the exciting part of this is.
REHMHow would that be a cure if you can target it before it shows if you have no cure for it after it exhibits?
KOROSHETZThat's a good question, and it turns out it's not -- it's actually a very insightful question because what is coming out from most of the research in neurodegenerative diseases is that if you wait too long, there are so many things that have gone wrong that it's really hard to reverse.
REHMDr...
KOROSHETZChances are early you're going to get it.
REHMDr. Walter Koroshetz of the National Institute of Neurological Disorders. Short break here. When we come back, we'll open the phones for your questions, comments. Stay with us.
REHMAnd here's our first email leading right out of the last issue we were discussing: "Is there a diagnostic test for early Parkinson's if one is experiencing constipation, restless leg and sleep issues?" Dr. Mari?
MARISo right now, we don't have a perfect diagnostic test which would have 100 percent specificity and 100 percent sensitivity. We do have some things to offer for an individual like that. The FDA recently approved an imaging technique called DaTscan. The DaTscan measures...
REHMHow do you spell that word?
MARICapital "D," lowercase "A," capital "T" and "scan"...
REHMOK.
MARI...one word. And this is a brain imaging that will image the dopamine transporter, which correlates with the dopamine neurons. It is expected to be abnormal even before somebody develops Parkinson's disease motor symptoms. These conditions that we discussed here earlier, the loss of smell, the REM behavior disorder or genetic positivity for the LRRK2 gene or constipation, and we can go on with this program on conditions. So they present before the motor symptoms appear. But it is assumed that the DaTscan would be abnormal, even before the motor symptoms appear.
REHMSo you no longer have to wait for autopsy to discover truly whether a person has Parkinson's. What about Alzheimer's? How does that fit in?
MARISo Alzheimer's would not produce an abnormal DaTscan. And as far as I know, these are prodromal conditions for the Parkinson's biology, are not prodromal for Alzheimer's. So there are some overlaps in how the disease mechanically develops, the biology of the protein aggregates and so on and so forth. But the clinical manifestations of Alzheimer's and Parkinson's disease will differ.
REHMAll right. And what about the relationship, Dr. Koroshetz, between Parkinson's and Alzheimer's?
KOROSHETZRight. So in both diseases, there's a common problem, and that is the nerve cells in the brain cannot process proteins normally. They can't get rid of them and metabolize them. So in Alzheimer's disease, inside the cell there's a protein called tau, and that aggregates and is associated with death of cells. In Parkinson's, the protein is synuclein.
KOROSHETZIt aggregates and is related to death of cells. So cells -- as people get older, these two problems kind of coalesce, and they potentiate each other. So in people who die late with Parkinson's, especially if there's cognitive changes, there's a high frequency that you're going to see Alzheimer's pathology as well.
REHMInteresting. Dr. Mapstone.
MAPSTONEYes. And there's a lot of overlap too with the notion that these are progressive diseases. And the idea is that these things move along at a specific pace and they can be exacerbated at certain times and maybe plateau at certain times. But it's a constant towards the death of these cells. And they produce different cognitive symptoms based upon where the pathology lies within the brain.
MAPSTONEAnd so this is why the cognitive profile of Parkinson's disease is really quite different from that of Alzheimer's disease, with the primary issue in Alzheimer's being a memory deficit typically, because the pathology resides in the area of the brain where memory is done. Whereas, on the other hand, with Parkinson's, the primary cognitive problem tends to be with these executive functions that we've been talking about.
REHMAll right.
MAPSTONEAnd that's because the pathology lives there.
REHMLet's take a caller in Myersville, Md. Noelle, you're on the air.
NOELLEHello, Diane. Thank you for taking my call.
REHMCertainly.
NOELLEI was wondering if your guests might comment on the possible link between infectious agents, like bacterial and viral infection, on Parkinson's and other neurodegenerative disease.
REHMDr. Mari.
MARISo there isn't a direct link. Parkinson's disease is not infectious. However, it is discussed in the context of infectious diseases in some ways. First of all, there's a theory that perhaps this aggregation of the synuclein that Dr. Koroshetz previously described could be following a mechanism similar to the prion diseases, the slow virus diseases, whereby a protein, such as synuclein, can assume two separate configurations in space -- one that's soluble and one and one is not soluble but it can aggregate. And then the bad one that aggregates gets in touch with the good one.
MARIThen somehow this property will propagate. And that's how we can see how it goes through the brain from the brainstem and then higher parts of the brain. And, if you will, that is sort of infectious, even though it's not going to be transmitted from one person to another. Another theory that relates some of these diseases with infections goes to the immune system.
MARIAnd when you have an infection you will produce antibodies. And there is some research showing that the antibody or immunoglobulin profile of Parkinson's patients or other movement disorders is quite specific. And maybe the antibodies play a role in some ways in the antiology of the disease, among the other factors we discussed.
REHMHere's an email from Oren in Alabama, who says he's been diagnosed with Parkinson's. "Please address stem cell therapy, which I am currently participating in." Dr. Koroshetz.
KOROSHETZWell, again, that's a really interesting topic. In the '90s, the NIH did fund a very major trial in stem cell replacement therapy in Parkinson's disease. The outcome of that trial is interesting. I believe, in my mind, it showed that the stem cells can be transplanted safely, that they do change the circuits and they do get rid of some of the symptoms of Parkinson's. The trouble is they kind of were uncontrolled and there was severe kind of increased movement that was a problem. So that trial was considered -- it just wasn't ready for primetime.
KOROSHETZNow, I think that there are people exploring new ways of doing this. Now, we can actually make stem cells from a skin biopsy from a patient. So these would not require any immune suppression to go back into the brain. So there's, I think, a new renewed interest in doing this, after we ran into severe problems with the first one.
REHMHow interesting. Dr. Mari.
MARII just would like to add on the topic of stem cells that, while it's very interesting and we have these barriers such as stem cells sometimes growing to tumors, such as teratoma and other problems that can occur with it, we have to keep in mind that, at best, stem cell therapies still are going to be symptomatic.
MARIWe are just putting dopamine factories in the brain, which is a much better way of delivering dopamine that's missing than our current ways of pills, et cetera. But you have to keep in mind that Parkinson's disease is not only dopamine. So even if you have the stem cell therapy perfected and the cells survive, they turn into dopamine producing cells and they do their job perfectly, even then, you are not as good as preventing Parkinson's that we mentioned earlier through the disease-modifying therapies.
REHMAll right. And a number of people are asking about essential tremors and how they differ from Parkinson's. I wonder, Dr. Mapstone, do you see an essential difference between essential tremors and Parkinson's?
MAPSTONESo certainly from a cognitive standpoint, these diseases do have different cognitive profiles. We tend to see fewer deficits in patients with essential tremor than in patients with Parkinson's disease. And the notion is, is that the underlying pathology in Parkinson's disease is more widespread and affects those cognitive or thinking areas of the brain more in a widespread fashion. So from a cognitive standpoint, we do see differences with fewer symptoms in essential tremor patients than in Parkinson's.
REHMBut I wonder whether essential tremor ever does move forward and develop into full-blown Parkinson's?
KOROSHETZWell, I'd say, you know, the vast majority of the people who have essential tremor are not going to get Parkinson's disease. There are a few people who begin with essential tremor as opposed to the usual Parkinson's tremor, which is called a rest tremor. And some of those people will go on. But that's, I think, a very small minority.
REHMAll right. Let's go to David in Marlborough, Mass. You're on the air, David. Go right ahead.
DAVIDWell, good morning and thank you. This is very informative. I'm a psychiatrist, and I've always, you know, distinguished between Parkinsonian side-effects, well, primarily the antipsychotics. But I also wonder about the role of psychiatric or other medications as risk factors for causing actual Parkinson's disease, and also about the reports that coffee consumption, two cups a day, may be somewhat protective. The other point that I have would be about...
REHMHow much coffee do you drink each day, Michael?
KINSLEYWell, I drink less than two cups. But I think I'll change that now.
REHMThe reports are coming out encouraging...
KINSLEYYes. And marijuana also is supposed to help.
KOROSHETZI don't know about that.
REHMWith Parkinson's? Dr. Koroshetz, you disagree.
KOROSHETZWell, I think we would -- I don't know that there's really firm data that marijuana prevents Parkinson's.
REHMOh.
KOROSHETZSo I think that needs to be studied, but the...
REHMPrevents or might alleviate symptoms?
KOROSHETZSome of the symptoms? Yeah, I, well...
REHMWhat do you think, Dr. Mari?
MARISo there are no prospective data that are strong on the topic. At the same time, we don't know. So without any good, highly powered prospective studies, we don't have the answer. What I usually tell my patients is that, you know, I'm not offering it or suggesting it. But at the same time, if it worked for them, I don't object.
KINSLEYNicotine also.
REHMNicotine...
KINSLEYIs, people say, helps the symptoms.
REHMAnd kills you of lung cancer in the process.
KINSLEYYeah.
REHMGo ahead, Dr. Koroshetz.
KOROSHETZThere are, as was mentioned, there are epidemiological studies that show that people who drink coffee have decreased risk of Parkinson's. People who have high uric acid have a decreased risk of Parkinson's. And then there were also studies that people taking a particular type of calcium channel blocker for their heart trouble had a lower risk. And NIH is now funding a trial of these calcium channel blockers in a prospective way to see if that's a true finding or it was confounded by other things in the epidemiology studies.
MARIAnd we are enrolling -- one of the enrolling sites. So people who are interested...
REHMGood. Excellent. All right, let's go to Iman in Chapel Hill, N.C. Hi, you're on the air.
IMANHi. Thank you so much for taking my call.
REHMSurely.
IMANLong-time listener, first-time caller.
REHMThank you.
IMANSo I'm a student at the University of North Carolina in Chapel Hill. And I'm a, you know, we're taking a neuroscience and a learning and memory class. And I was wondering if reducing risk for other neurodegenerative disorders can also help reducing risks of Parkinson's disease, for example, you know, because the two can often be found comorbid with each other and developing, not necessarily at the same time, you know, they can be present in the same person. So I was wondering if there are -- if it's being researched separately, like Parkinson's and Alzheimer's, or are they ever -- do they ever get researched together, you know?
REHMAll right. Dr. Koroshetz.
KOROSHETZWell, again, a good question. I think a lot of people are researching these neurodegenerative diseases as a single entity with different flavors. So that is indeed happening. In terms of what you can do to prevent, it's a little harder to know. But I think the evidence that's out there now is that one of the most trophic things for the brain is exercise. So exercise is seemingly great for your muscles but probably better for your brain.
REHMMichael, you were a runner, it seems to me.
KINSLEYWell, I've never been -- certainly, growing up, I was no athlete. But since I've been diagnosed, I take exercise very seriously. And I think, if I had to choose between exercise and the drugs, I would choose exercise.
REHMAnd you're listening to "The Diane Rehm Show." So how much time do you devote to exercise, say daily?
KINSLEYAn hour.
REHMAn hour?
KINSLEYYeah.
REHMGood for you. And is it running, or is it stretching or walking?
KINSLEYOver the years, I've tried running, then -- you know, you're not exempt from all the other terrible things that happen as you get older. So my knees start to go if I run too far.
REHMOf course.
KINSLEYBut -- and I, you know, the weight machines and whatever is available at the gym.
REHMOf course I am a huge believer that walking is the ideal exercise for all of us and does avoid the knee problem. Go ahead, Dr. Koroshetz.
KOROSHETZJust on this point, the NIH funded a trial, which you'll find interesting. It was a trial of Tai Chi, a particular type of exercise. And that actually showed benefit and it was published in the New England Journal about two years ago. So I think there is something about exercise. I don't know, Michael, do you feel better when you exercise?
KINSLEYOh, yeah.
KOROSHETZYes. So there's a very acute effect that people with Parkinson's notice with exercise.
MARIIt may reduce the needed medication levels as well in some. And of course, long-term, it has benefits. People who have a good exercise schedule typically do better. And we don't know if it's a conditioning effect or in fact it is a direct effect on the brain. But at this point, I don't really care as long as they are better.
REHMBut I want to be clear with our listeners. Currently, there are no biomarkers for Parkinson's. Is that correct?
KOROSHETZWell, I think, you know, we were talking about the DaTscan.
REHMYeah.
KOROSHETZSo that is, in a sense, a biomarker that reflects the dopamine problem.
REHMBut has it been used over and over again?
KOROSHETZYes.
MARISo it has been used clinically. The FDA approved it as a standard clinical procedure in 2011. And it has been used ever since then in clinical practice. What we are trying to do through some research funded by the Michael J. Fox Foundation is to see if we can do better than just, yes, abnormal, no, normal, but quantify it and use it as a biomarker in terms of how severe the loss is. And this would be one of the potential progression biomarkers.
REHMAnd one last, quick email. "My dad used to putter around the house," says Zen, "and used benzene like it was water. He's cleaned his tools, hands with it. He inhaled fumes. Clearly that contributed to both his diagnosis of NHL." What is that? Anybody know what that means?
KOROSHETZI don't know.
KINSLEYNational Hockey League.
KOROSHETZThat's right. Yeah.
REHMAnd Parkinson's disease, would you agree, benzene could, indeed?
MARII don't believe it could be a single cause and just by itself. I believe that some people could be susceptible to Parkinson's because of genetic predisposition. And a variety of environmental factors, including toxins, could then cause it in context with that.
REHMAll right. And I'm afraid we've got to leave it at that. Dr. Zoltan Mari, Dr. Mark Mapstone, Dr. Walter Koroshetz and Michael Kinsley...
KINSLEYNot a doctor.
REHM...not a doctor, but a man who is living through some very important medical issues. Thank you all so much. Thanks for listening. I'm Diane Rehm.
After 52 years at WAMU, Diane Rehm says goodbye.
Diane takes the mic one last time at WAMU. She talks to Susan Page of USA Today about Trump’s first hundred days – and what they say about the next hundred.
Maryland Congressman Jamie Raskin was first elected to the House in 2016, just as Donald Trump ascended to the presidency for the first time. Since then, few Democrats have worked as…
Can the courts act as a check on the Trump administration’s power? CNN chief Supreme Court analyst Joan Biskupic on how the clash over deportations is testing the judiciary.