Diane’s farewell message
After 52 years at WAMU, Diane Rehm says goodbye.
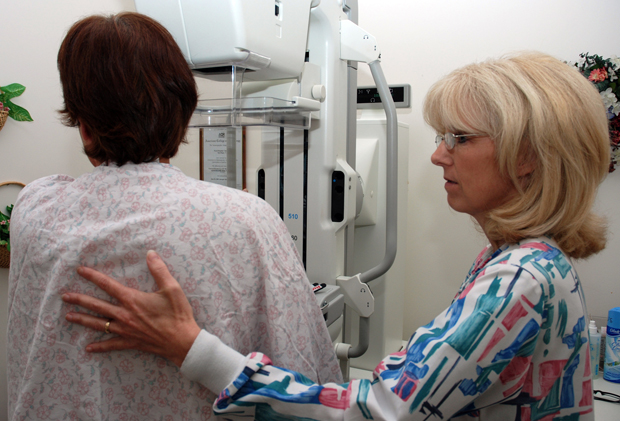
Lead Mammography Technologist Carmen Waters assists a patient preparing for a mammogram.
A new study about a form of early-stage breast cancer called ductal carcinoma in situ (D.C.I.S) has left women as confused as ever about how to treat it. Up to 60,000 American women a year are told they have DCIS; most opt to have a lumpectomy or mastectomy, but many women choose to have both breasts removed, even if one breast shows no sign of DCIS. Some cancer experts say the study offers more evidence that we’re over-treating women. Others say DCIS should still be viewed as potentially dangerous and treated aggressively. We look at the latest research and what it means for patients.
MS. DIANE REHMThanks for joining us. I'm Diane Rehm. Up to 60,000 women a year are diagnosed with an early stage of breast cancer known as DCIS. As technology improves, it's showing up more often on mammograms. Most women who get the diagnosis decide to have some form of surgery, but a new study raises questions about whether early treatment changes outcomes.
MS. DIANE REHMHere to talk about DCIS, Dr. Barnett Kramer of The National Cancer Institute. Joining us by phone from Washington, breast cancer surgeon, Dr. Shawna Willey of Georgetown University's Lombardi Cancer Center and from a studio in Portland, Oregon, Dr. Vinay Prasad, an oncologist who specializes in patient decision-making and health policy.
MS. DIANE REHMI know many of you will want to join us. We've got to have clear information on this issue and I hope we can give it to you this morning. Join us, 800-433-8850. Send an email to drshow@wamu.org. Follow us on Facebook or send us a tweet. And thank you all for being with us.
DR. BARNETT S. KRAMERThank you. It's a pleasure to be here, Diane.
DR. VINAY PRASADThank you, Diane. Thanks for having me.
DR. SHAWNA WILLEYThank you very much.
REHMGood to have you all. Dr. Kramer, start by explaining just what DCIS is.
KRAMERDCIS is a shortened form of the longer term, ductal carcinoma in situ. And DCIS, largely these days, is diagnosed almost exclusively by mammography. It has a characteristic picture on the mammogram and therefore is frequently picked up by mammography. The controversy involves what it actually means. Many of the lesions are probably related directly to cancer and precancerous and would move on to cancer, but much, much larger proportion of them we don’t know the natural history.
KRAMERAnd emerging information, such as the data that came out of the most recent paper (word?) oncology suggests very strongly that the overwhelming majority of them may not progress.
REHMDr. Prasad, what does this study indicate to you?
PRASADWell, Diane, the study that Dr. Kramer's talking about is an observational study and so what the researchers did in this study was they looked at 100,000 women with DCIS and they followed them for many years in a national registry. And observational studies are great to tell us things like how worried we should be about some bad event happening to us, but observational studies are also a little bit difficult in telling us what we should do because all of the women in these studies, they only did one thing.
PRASADThey did what had happened to them. So I think some people will read this study, which shows, in general, that women with DCIS have a low risk of having a breast cancer in the future and have a very low risk of dying of breast cancer, in fact, identical or very similar to people who didn't have DCIS. And there would be -- there's no difference from certain treatments. Some people would look at this as saying that this is sort of an indication that, you know, we're doing too much.
PRASADWe're over treating. We've over diagnosing this problem. Others might say that the reason the outcomes are good in this study is because of what we're doing and so I think, for this particular study, can kind of be interpreted both ways.
REHMSo your personal interpretation would be what?
PRASADSo my interpretation, and this is based not just on this study but on all of the randomized trials we've conducted, is that this study shows pretty convincingly that some of the treatments we're using for these women, for instance, the addition of radiotherapy after lumpectomy, that that doesn't confer a very large benefit and possibly, you know, no benefit at all from that particular intervention.
PRASADAnd mastectomy and double mastectomy, these are choices that women are making and I think this study suggests that those choices, you know, they may be right for some women, but for other women they may be too much.
REHMAnd to you, Dr. Shawna Willey, will this study change recommendations you give to breast cancer patients?
WILLEYWell, I think we need to take into account all of the data that is available to us and I certainly expect that patients will be asking me about this study. One of my concerns about a study like this is that the results will be generalized to all patients with DCIS. And because DCIS is really not just one disease, it's a heterogeneous group and in this study they showed that women younger than 35 or women with specific kinds of DCIS actually had a higher mortality than all of the rest of the patients.
WILLEYSo I have to take all of this into account when I counsel a patient and I have to look at what the individual characteristics of the patient are, as well, as the individual characteristics of their DCIS so that I can make a good recommendation to them about the amount of treatment that they need or whether they could have watchful waiting as an option.
REHMNow, explain to me how a mammography can indicate specific kinds of DCIS on which you would then base a judgment.
WILLEYWell, when a woman has a mammogram, as was already mentioned, there is a characteristic appearance of calcifications and the vast majority of DCIS now is diagnosed by a core needle biopsy, which should be the first intervention and the way a biopsy -- or the way a diagnosis is made. The calcifications are relatively easy to see on a mammogram, although they are very small and they tend to cluster. So we cannot say exactly what something is based on its appearance on a mammogram.
WILLEYWe can see if there's a probably of that appearance being cancer, but then we need to follow that up with a diagnosis or with a biopsy that gives us a very specific diagnosis by looking at that tissue under a microscope.
REHMSo from your perspective, this study would not lead you to tell women, for the most part, to watch and wait if DCIS is discovered by mammography.
WILLEYIf we diagnosis DCIS on a core needle biopsy, the usual recommendation is to remove that area so that we get clear margins. And what that means is that we need to remove the tissue so that all of the cancer cells have been removed or at least all those that were visible on the mammogram. Now, there are some studies being designed to actually watch patients without having surgery.
WILLEYSo the diagnosis is made by a needle biopsy. We know what kind of cancer they have and we may not put them in a category of those high risk lesions. And those patients may be offered observation. But, in my opinion, we need to design those trials and watch those patient very closely so, first of all, we aren't harming patients and second of all, we're going to get the most information from those kinds of studies.
REHMDr. Prasad, from your perspective, what would be the risks of having surgery, either a lumpectomy, a mastectomy or even a double mastectomy versus the risk of doing nothing?
PRASADThat's a very good question. So I think that certainly the risk of surgery increase with the extent of surgery and a double mastectomy or a mastectomy are much more disfiguring surgeries than a lumpectomy alone. The decision to -- among those three options, they've -- it's historically been based on the amount of DCIS and what the surgeon thinks is feasible. Many women feel scared or pressured or that the best decision is just to go ahead and remove this problem entirely and have the lumpectomy -- and have the mastectomy.
PRASADAnd that decision is, of course, a personal one, but is one that this study does provide some information suggesting that the likelihood of a breast cancer recurrence, even with the lumpectomy is very low. The additional benefit of having the full mastectomy that is even lower than previously thought and that's not that benefit in terms of breast cancer survival or the most important end point, how likely a women is to die of breast cancer.
PRASADSo I think that information is empowering to women to make a choice that's right for them.
REHMSo Dr. Kramer, how come we're discovering so much more DCIS now than in the past?
KRAMERPrior to the mammography era, it was very rare diagnosis so this really is a diagnosis that comes from mammography. Prior to the mammography era, there were somewhere between 600 and 700 cases a year. Now, there's somewhere in the neighborhood of 55,000 cases a year. So the incidence of DCIS has gone up perhaps 100 fold. And the stakes are high as -- and I just mentioned for the individual woman because the treatment options carry with them very different side effects.
KRAMERSurgery itself, lumpectomy itself hopefully will preserve the cosmetic appearance of the breast, but not always because women who have small breasts are going to have worse cosmetic outcome. But once you start adding things -- interventions like mastectomy, the side effects become much worse. And it's not just the cosmesis. As a matter of fact, breast reconstruction has a long recovery period.
KRAMERIt requires exercising to recover the strength that is lost and many women will never recover all the loss of strength and they may not be able to participate in sports like they used to, specifically, tennis, golf, things like that.
REHMDr. Barnett Kramer, he's director of the division of cancer prevention at The National Cancer Institute. Short break. Stay with us.
REHMAnd welcome back. We're talking about a new study regarding breast cancer, specifically DCIS, an early stage of breast cancer and it's showing up more often on mammograms. Women who get that diagnosis tend to want to have treatment, either a lumpectomy, a mastectomy or even having both breasts removed. And studies somehow are confusing here, Dr. Kramer. Tell us what the outcomes are. Can the idea of removal of a lump or a breast -- can that somehow indicate or cause cancer to spread to other parts of the body?
KRAMERAs far as we know, the surgery itself does not need to spread. The key question from this study and others -- because as Vinay earlier mentioned, there are actually several randomized, controlled trials that support what I'm about to say -- do not seem to suggest that what you do locally affects the risk of spread. And for DCIS, the risk of spread is already very, very low. One investigator has even said, welcome to the world of very low probabilities. No matter what is done locally, the outcome appears to be quite good. There are subsets of women with DCIS who have a worse prognosis and at least, as a first approximation, we basically know who they are.
KRAMERFor example, in this study, women who are under the age of 35 had a higher risk of dying of breast cancer, irrespective of the treatment they received to that breast. But that only accounted for less than 1.5 percent of all diagnoses of DCIS in the country. So it's a small subset. We can already identify some of those subsets. But it's for the vast majority, where the stakes are so high and we struggle: Should we give radiation therapy? Should we do a mastectomy? Should we do a double mastectomy? Radiation therapy has its own harms as well. It is known to cause cancer subsequently in people. Radiation is a proven human carcinogen. And sometimes women will get tamoxifen, a hormonal treatment, and tamoxifen is also known to be a human carcinogen.
REHMSo it leaves women with DCIS really in a confused area.
KRAMERYes. So informed decision making is a very important issue. As the evidence accumulates, I think it's our obligation to tell women, individually, exactly what we know and what we are learning and participate in the decision. But, ultimately, they need to know what the potential benefits are, but also what the harms are. And there are clearly some harms that they will have to suffer if they choose one therapy versus the other. It's reassuring to be able to tell them that amongst the most commonly used treatments there doesn't appear to be a real difference, so it's mainly the side effects and the harms of therapy that may weigh more heavily in their decision.
REHMDr. Prasad, do I understand correctly that, even if a woman does have a lumpectomy or a mastectomy, that cancer may show up in other parts of the body?
PRASADThat's correct, Diane. One of the interesting things about this present paper was that the authors found that about half of the women with DCIS who ended up having a metastatic spread of breast cancer -- breast cancer that's spread outside of the breast -- half of them had -- they first had the breast cancer recur in the breast. But the other half had the breast cancer just occur in the periphery, without having first occurred in the breast again, suggesting that we don't fully understand how this spreads and how this progresses.
PRASADBut just to bring one point up, you know, what has widespread mammographic screening done for DCIS and what has it done for advanced cancer? Well here's some numbers that came out recently. You know, in the 1970s, we had about 110 women per 100,000 women were diagnosed with either early breast cancer or DCIS. That number today is now 234. It's more than doubled. And that doubling would be justified if we were reducing the rate of advanced cancer -- cancer that's spread outside of the breast or at other parts of the body. But that number has changed only from 102 to 94, a very small change and not proportionate to the huge burden of breast cancer we're seeing.
PRASADAnd many researchers, Dr. Kramer and myself and other researchers believe that this represents a phenomenon called "over diagnosis." That this -- there's breast cancer that exists that we would never have detected in a woman's lifetime but because we're more aggressively looking for it, we're catching these small tumors. These are tumors that women would never have felt, they never would have bothered them. And treating these tumors adds considerable harm without even the possibility of benefit to treat an over diagnosed tumor. And the question of course is, on average, are you benefiting these women? And I think that's the tough question of DCIS.
REHMSo, Dr. Willey, how would you respond to the idea that there is over diagnosis here?
WILLEYWell, I actually agree with that statement. But I think the challenge in this setting is that we have a population-based study that shows these results, and yet, on a daily basis, we have women who are faced with this diagnosis. And we, as clinicians, and the patients, as patients, have to make decisions about how they're going to deal with this information. I think there's a tremendous amount of fear around the diagnosis of breast cancer. And that whole controversy about whether DCIS even represents breast cancer as an entity remains a controversy.
WILLEYAnd so the confusion for the individual patient -- the patient who's sitting down in my clinic right now, waiting to discuss DCIS -- is a very confusing situation, when they hear headlines like this that say we're over treating all DCIS. So we have to be careful how we communicate, both as physicians to our patients and as, I believe, media to the patients. Because I think there's no one on this call who would say that no one needs to be treated for DCIS.
REHMRight. But the question becomes, the risk of doing something versus the risk of doing nothing, Dr. Willey.
WILLEYThat's exactly right. And that's where some of these controversies come in. One of the things about this study is it's very surprising that there was a group of patients who developed cancer in other parts of their bodies when we generally define to the patients that ductal carcinoma in situ cannot spread. So there are limitations that we have as far as the pathologic analysis and predicting the biologic behavior of these cells. And we know, again, that there's a very heterogeneous group here. The trick for us, as clinicians and researchers, is to do more studies to figure out, which ones could we safely watch and which ones need more aggressive treatment?
WILLEYThat's happened with all kinds of cancers. And there's certainly some cases of DCIS where watchful waiting is absolutely the best choice. But our limitation right now is to pick those patients out from the whole group and give them the right answer as far as how they should be treated.
REHMBut, Dr. Kramer, you seemed to indicate earlier that you can separate out those with DCIS who need no treatment from those who need more aggressive treatment. Surely, age has got to be one factor.
KRAMERAge is an important factor, albeit the diagnoses of ductal carcinoma in situ, DCIS, that occur in very young women are generally not through mammography. And so even within this study, there's a suggestion that mammography identifies a particularly slow-growing or non-growing form of DCIS.
REHMA zero form.
KRAMEROf stage zero. But no matter what the DCIS is, I don't think we can reassure anyone that there's no chance whatsoever, a zero probability of progression. But this type of study gives us confidence that the choice of therapy may not play a large role in the ultimate outcome. And that -- this is simply a study that is observational and not a randomized trial. There's very large numbers in this study and it does support randomized trials that have come before it.
KRAMERDr. Willey said some -- two things that are very important and I want to emphasize. Number one, the woman needs to know what we know and what we don't know -- what we wish were true, but what we don't know. And when we don't know, we have to be very honest about it. And the woman can help us decide what is the most appropriate therapy, since she bears the consequences, both good and bad. And then, finally, we can't stop here. We have to build on the information that we have. And these types of studies are helping us justify watch-and-wait studies.
KRAMERI'll point out the parallel with prostate cancer, where there was a huge increase in diagnoses of prostate cancer simply as a result of screening efforts with PSA. Over time, we learned that a lot of PSA-detected cancers were very slow growing and best left alone. And that started to justify studies which were purely watchful waiting, after a needle biopsy. And now I think we're starting to build the evidence base to justify that. We may not be there, but I do think that this type of evidence helps us justify studies such as that.
REHMDr. Prasad, I'm sure family history would very much figure into decision making, once DCIS is discovered.
PRASADSo, I think a couple things we've talked about as sort of the things that came out of this recent study as kind of concerning. One was the women younger than 40. But as Dr. Kramer makes a point, because we don't normally have mammographic screening for those women, likely their cancer is detected differently. They may have had a bloody nipple discharge or some other cancer sequelae. It may be a different sort of DCIS. The other thing that jumped out of this study was race. African-American women had much higher rates of breast cancer death. That's something we've seen time and time again.
PRASADThe role family history plays is very varied. Of course, there are some familial cancer syndromes, mutations in certain genes. We know those confer extremely high risks of breast cancer and breast cancer death. And studies suggest that even prophylactic mastectomy may have some benefit at those levels of risk. But in this particular case, I think, for DCIS and the sort of average family history, I think that's a little bit more difficult to tease out the -- how much that should sort of change your decision making.
REHMHmm. Suppose a young women has, say, a double mastectomy, because she discovers, through mammography, DCIS. Say, a woman 35 to 40. Is a double mastectomy there warranted, if there is no family history? Dr. Kramer.
KRAMERYeah, so, number one, that's rather intense, extreme therapy. And I think that we have enough evidence from studies like this and other studies that a double mastectomy would not change the outcome.
REHMBecause?
KRAMERBecause the risk of dying of breast cancer is virtually identical, whether the woman has a lumpectomy, lumpectomy with radiation, single mastectomy or double mastectomy.
REHMHow can that be, if the breasts are removed?
KRAMERWell, the one thing I've learned over my career is that science, in general, and medical oncology science, in particular, is highly counterintuitive. But we are learning that there is an element of biological predeterminism -- that is, the characteristics of tumor cells at the time of diagnosis -- may determine the outcome more than what we do locally with that tumor.
REHMAnd you're listening to "The Diane Rehm Show." Can you say more about that? I'm not clear about what you mean.
KRAMERYes. So one of the clearest demonstrations in this study was what Dr. Prasad said. And that is, of the women who ultimately died of metastatic breast cancer, actually more than half of them, about 54 percent, had never had a recurrence of the tumor in the breast -- the original breast. It just appeared for the first time as metastatic disease. And the other half, or about 45 percent, did have a recurrence in their breast.
KRAMERAnd that's an indication that what was done at the outset -- or reinforces the information that came from the larger study -- that the choice of therapy and what was done locally had little to do with the ultimate outcome. And of course the most feared outcome is metastatic spread and it does not appear that what was done locally affected that.
REHMSo even removal of the breasts, even radiation, even chemotherapy does not stop the metastasis of that cancer that originated in the breast.
KRAMERYes. Now, as Dr. Prasad said, this is not a definitive study. No study is definitive all by itself. That's why I've mentioned other randomized trials. But it does give a suggestion. And, remember, virtually all these women had some treatment. They either had a lumpectomy, with or without radiation, or a mastectomy, or double mastectomy and some of them had tamoxifen.
REHMLet's talk also, quickly, about older women...
KRAMERYeah.
REHM...my age. Women in their 70s.
KRAMERYes.
REHMSuppose I were to discover a DCIS at my age. I would be less than inclined to do anything about it.
KRAMERYes. And that raises an extremely important point about the complexity of individual decision making. Because the older a woman has -- the older a woman is, the more she has to think about, when do the side effects occur? If this -- in an 85-year-old woman, obviously, the side effects occur early, the side effects are front loaded, and the benefits may only be theoretical.
REHMAll right. We'll take a short break here. And your calls, your comments, when we come back. Stay with us.
REHMAnd here's our first email from Taras. She says autopsies of old women who live long and without cancer have hundreds of lumps. For that matter, lumps have been there throughout life and have done no harm. The existence of a lump demonstrates the body's ability to encapsulate cancerous cell growth. Lumps are good. How do you feel about that, Dr. Prasad?
PRASADWell, I'm not sure I will agree with everything in that email, but I will say that one of the things that the email sort of gets at is this idea that there are some cancers for which the biology is so slow-growing, so docile that women do die of some other reason, and on autopsies we discover that these cancers are present. That's also particularly true with prostate cancer as men get older. They say that for every decile of age, you have about a 10 percent increased risk of having some prostate cancer detected.
PRASADAnd I think that what that's getting at is this idea of over-diagnosis, that some of the cancers that we're finding and treating are cancers that otherwise would've gone undetected. And then the question becomes, is the net harm that's being done to the over-diagnosed cancers outweighed by the benefit being granted for the cancers that really would cause problems. And that's always the balancing act in early breast cancer studies.
REHMAll right, let's go to the phones, first to Patricia. She's in Cincinnati, Ohio. Go right ahead, Patricia.
PATRICIAThank you so much for taking my call.
REHMSurely.
PATRICIAI was diagnosed with DCIS when I was 35 years old, in 1996. I had a lumpectomy and radiation therapy. My cancer was quiet until 2010. When my breast cancer returned, I had a mastectomy and a latissimus flap reconstruction. But before that, in 2008, I was diagnosed with a massive tumor, a liposarcoma, in my retroperitoneum. So my two -- my one question is, could the radiation have affected the development of liposarcoma in my pelvic retroperitoneum area? And the second is, the latissimus flap reconstruction, I totally disagree with the physical, that one doctor who said something about coming back from these kinds of reconstruction are difficult. I was doing butterfly in the swimming pool literally three weeks after my surgery. As soon as I was allowed to get in the pool, I was in the pool. I'll be quiet now and take your response. Thank you very much.
REHMAll right, thanks for calling. Dr. Kramer?
KRAMERWell, first of all, I'm very glad to hear that despite the flap and -- the muscle flap that you were doing well and can participate in all of your exercises. However, that's not always the case. And I certainly have personally spoken to a number of women who complain that they do have the side effects of surgery, and they do persist. But importantly, back to your issue of could the radiation to your breast have caused the abdominal tumor, the chances of that are very, very likely. It probably is not the cause because when radiation therapy causes secondary malignancies, it's within the port, it's within the area that the radiation hit.
KRAMERSo it wouldn't be surprising to find a sarcoma of the chest wall or the underlying bone or of the lung, but it would be very surprising if it caused an abdominal tumor.
REHMAnd joining us now by phone from Massachusetts, Dr. Daniel Kopans. He's professor of radiology at the Harvard Medical School. Thanks for joining us, sir. What are your thoughts on the new DCIS study and the interpretations?
DR. DANIEL KOPANSWell, Diane, thank you for having me on.
REHMCertainly.
KOPANSI have to say it's been a little frustrating listening and not being able to say anything. I think it's very, very important, and we all agree, that women need accurate information. The first thing I'd like to point out, and Dr. Kramer touched on this, this paper that we're discussing says nothing about watchful waiting. It says nothing about that you can leave ductal carcinoma in situ alone and not treat it. Everyone in this study was treated, either with a lumpectomy, which I would assume was taking out the tumor and, as best the pathologist can tell, there's no tumor left in the breast. Now that's a bit of a guess to a certain extent, but the tumor was completely removed, or the tumor was removed with radiation or, and we've heard the different, you know, mastectomy scenarios.
KOPANSSo this paper can't be used to say it's safe to do nothing about ductal carcinoma in situ. What it does say is that the therapy to the breast doesn't seem to alter the ultimate survival. It probably, if you treat the breast, if you at least take the tumor out, that saves lives, but you may not save more lives by adding radiation and/or more surgery with mastectomies. And that's been shown actually in invasive cancers. The treatment to the breast is primarily to prevent recurrences in the breast. And years and years ago, it was shown that if you took the tumor out, or you took the tumor out with radiation, or you did a mastectomy, survivals were the same for invasive cancers. So number one, this paper doesn't say that watchful waiting is safe.
KOPANSNumber two, the comment was made that there's a lot of over-diagnosis. Certainly ductal carcinoma in situ is an area where we all agree we don't know who really needs treatment and who doesn't, and unfortunately this paper doesn't actually shed any information on that, but we do know that invasive cancers found by mammography and other ways are invasive cancers, and they will kill you if left alone.
KOPANSI would challenge anyone on this call to tell me that they have seen an invasive breast cancer disappear on its own, without treatment, and I will take the guess that no one has ever seen that because there aren't any credible reports even in the medical literature of this happening. The papers that say that there's a lot of over-diagnosis of invasive cancers have all been disputed and shown to be scientifically incorrect.
KOPANSAnd the other point that I would make in terms of the paper itself is that, as has been pointed out, this was not a randomized trial. This was a retrospective review of what happened to people. And the question is, why were the various women treated in various different ways. My guess would be that the women who just had a lumpectomy probably had a very small tumor, and it was felt by the oncologist that if you just took it out with hopefully a wide margin of normal tissue that that would be sufficient, and then for larger tumors or perhaps histologically, under the microscope, tumors that looked more aggressive, they recommended adding radiation, and then decisions for mastectomy are usually based on the size of the tumor.
KOPANSSo these -- the tumors in these three categories of treatment were almost certainly different tumors. So it's very hard to say that treatment makes absolutely no difference. It made no difference based on the way these women were separated into treatment groups. Another point that I would make, and I am the radiologist on the call, we can't tell ductal carcinoma in situ apart, the different kinds of ductal carcinoma in situ, apart on a mammogram. There are some that -- most of them, as was correctly stated, are found by seeing little calcium deposits on a mammogram, but the radiologist generally can't say, oh, that's a low-grade or intermediate- or high-grade.
REHMAll right.
KOPANSAnd the other point is that some of the calcifications that we find, people have said, well, why don't you just ignore all the calcifications so we don't have to deal with DCIS, and the problem with that is about 15 percent to 20 percent of invasive cancers are detected because of the calcifications in the part of the tumor that is still DCIS. So DCIS is almost certainly the precursor, the lesion that comes first, before an invasive cancer, and sometimes what's left of the DCIS gives way to the presence of the invasive cancer. But...
REHMAll right. I think -- I think that Dr. Kramer may have some comments, especially on the statement that the treatment of breast cancer and most especially DCIS saves lives.
KRAMERYes, certainly one can look to this study to document that, but it is certainly true that, as Dr. Kopans said, virtually all these women get treated. I think it's a matter of speculation, and I wouldn't guess exactly which women got therapy, since that's in the study, and what decisions went into the decision on the part of the woman and her surgeon to go one way or the other. That's simply not in the study.
KRAMERIt is certainly true that they all got, or virtually all got, some form of therapy. But as I pointed out earlier, this is not a definitive study. We have learned from this study, however, that the vast majority of these -- of DCIS, do just as well, probably, with either lumpectomy or with or without radiation mastectomy, double mastectomy, and this sets the stage, just like it did in prostate cancer, screen-detected tumors, for doing studies on watchful waiting in which a needle biopsy is done, and no subsequent therapy is done, even for some classes of what appear to be slow-growing invasive tumors.
REHMAll right, and here's my question for you, Dr. Kopans, and I'll ask it of others as well. I don't know if you're married or if you have a daughter, but if you did have a wife, and it was discovered she had DCIS, what would your recommendation be for her?
KOPANSWell, I unfortunately don't have a daughter, I have two sons, but I have daughters-in-law, and I have two granddaughters. I would probably go with lumpectomy and radiation, but I would rely on my oncology colleagues to advise her and advise us. I think that it's again important to reiterate that we don't really know that we can leave these tumors alone. I would agree with Dr. Kramer that if we can study it, that's great, but at the Harvard teaching hospitals, we actually tried to reduce the amount of treatment by taking early grade one and intermediate grade two DCIS, so the theoretically lower-risk lesions, and small ones, and we did a wide excision. That meant we took the tumor out, and as far as the pathologist could tell, there was at least a centimeter of normal breast around the DCIS, and then we did nothing else.
KOPANSPatients were informed, and they agreed to do this. And we had to stop the study because the recurrence rates were too high. They were 12 percent at five years, and 30 percent of those were invasive, and when DCIS comes back as an invasive cancer, as this paper shows, it's a much bigger concern.
REHMBut...
KOPANSThe reason for treating the breast is to try and prevent recurrences. That's the primary reason for treating the breast for all cancers, but clearly this paper shows with DCIS, systemic treatment hopefully kills, if you give chemotherapy for example, kills tumor cells that may have already gotten out. So clearly in some of these women, the tumor cells had become invasive, had gotten out of the breast and had metastasized. We actually don't know whether they recurred in the breast or not because we don't know if all the women got mammograms to see if they had come back.
REHMAnd you're listening to the Diane Rehm Show. Dr. Prasad, do you want to jump in here?
PRASADSo I think your question was how would you advise someone who is a loved one. I think the first thing I'd say is of course there's no single right answer for everyone, and the choice is ultimately up to your loved one, up to the woman. And then I'd say that, you know, the way -- doctors tend to be conservative, and so all doctors would recommend at least some surgical treatment, probably a lumpectomy or something else.
PRASADIf -- there are studies that are ongoing that are comparing watchful waiting to a lumpectomy right away. If that study was available to a woman, I would say that that's always a great option, to participate in a clinical study. Those exist because don't know the right answer, and it can possibly some morbidity. Then the question becomes the addition of radiation therapy. And we know from this study that about 20 women have to undergo radiation so that one is spared a future breast cancer -- invasive breast cancer and that there is no breast cancer overall mortality from that.
PRASADAnd that's a decision that really is an individual decision, whether or not that risk is worth the benefit, and that's sort of how I would advise a woman.
REHMDr. Kramer?
KRAMERYes, I'll just reinforce what Dr. Prasad said. Adding radiation therapy is not without its consequences because we can be confident that there'll be an increase in tumors, malignant tumors, after we've delivered radiation, and a woman obviously has to know that, and the risk starts to increase after about seven or eight years and continues to rise. But Dr. Prasad said that it really is a personal choice. If there's a study, that's important, and I would only point out that everyone has pointed out the weaknesses and warts in the JAM oncology study, but it's even more difficult to interpret definitively a study that comes out a single tertiary referral center because a different type of patient may be coming.
REHMSo let me ask you the same question I asked Dr. Kramer. If it were a beloved relative, what would you say to her if DCIS were discovered?
PRASADWell, as I hinted before, my tack would be very similar to the one that Dr. Prasad just took, and that is we need to tell the woman what we know and what we don't know and talk to her about what we know about benefits but also what we know about harms of all of the choices. I think that if the biopsy does not show any of the dangerous characteristics that sometimes appear even in DCIS, for example there's a characteristic picture under the microscope as described in the Lancet oncology paper, that predicted a higher rate of recurrence.
PRASADBut if you don't see that, I think that you would take all the woman's characteristics together. I don't have -- I have a wife. I don't have any daughter, unfortunately. I'm in the same boat as Dr. Kopans. But if I did, and with my wife, I would go through the type of reasoning that Dr. Prasad just did.
REHMAnd would you necessarily do a biopsy?
PRASADWell, that is a matter of growing controversy. Dr. Kopans mentioned that there are some investigators out there who would say the target for screening should not be micro-calcifications, it should be other characteristics, other than those that are the hallmark of DCIS. That is highly controversial, and for that I actually defer to the radiologist's call, but it's also worthy of study.
REHMAll right, and we are out of time. A great discussion, thank you all. Dr. Barnett Kramer, Dr. Shawna Willey, Dr. Vinay Prasad and Dr. Daniel Kopans. Thanks for listening, all. I'm Diane Rehm.
After 52 years at WAMU, Diane Rehm says goodbye.
Diane takes the mic one last time at WAMU. She talks to Susan Page of USA Today about Trump’s first hundred days – and what they say about the next hundred.
Maryland Congressman Jamie Raskin was first elected to the House in 2016, just as Donald Trump ascended to the presidency for the first time. Since then, few Democrats have worked as…
Can the courts act as a check on the Trump administration’s power? CNN chief Supreme Court analyst Joan Biskupic on how the clash over deportations is testing the judiciary.