Diane’s farewell message
After 52 years at WAMU, Diane Rehm says goodbye.
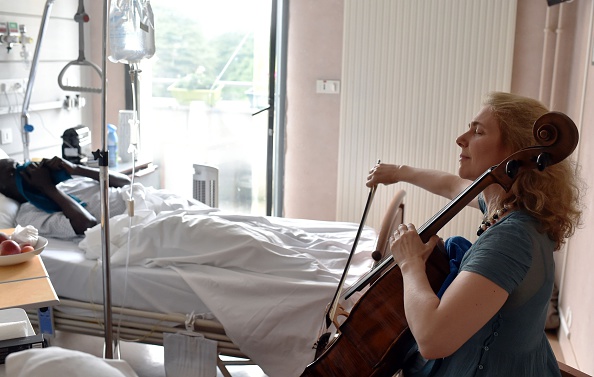
French musician and art therapist Claire Oppert plays music for a patient at an intensive care unit of the Sainte Perine hospital on July 11 in Paris.
Music therapists have been working to help patients for decades. In recent years, research on music and the brain has indicated listening to songs can help patients with a wide range of medical problems, including sleep disorders and strokes. Classical guitarist Andrew Schulman says music helped him recover from a coma. While he’s not a music therapist, he now works with doctors in intensive care units at Mount Sinai Beth Israel hospital in New York and Berkshire Medical Center in Massachusetts. He plays his guitar to help stabilize patients blood pressure and heart rates after surgery. A look at how music is being used to aid patients recover from medical conditions.
Excerpted from WAKING THE SPIRIT by Andrew Schulman, with an Afterword by Marvin A. McMillen, M.D., FACS, MACP. Published by Picador. Copyright © 2016 by Andrew Schulman. Afterword copyright © 2016 by Marvin A. McMillen. All rights reserved.
Waking The Spirit by wamu885 on Scribd
Watch a preview of Dr. Patel’s “Music and the Brain” class. You can learn more here.
MS. DIANE REHMThanks for joining us. I'm Diane Rehm. Scientific studies show that listening to music could help patients recover from surgery, alleviate pain and treat sleep disorders. Here with me to talk about what research on music and the brain could mean for medical treatment, Andrew Schulman, author and professional musician and Dr. Marvin McMillen with the Berkshire Medical Center in Massachusetts.
MS. DIANE REHMJoining us by phone from New York City, Connie Tomaino with the Institute for Music and Neurologic Function, from a BBC studio in Nottingham, Britain, John Powell, author, scientist and musician and from WGBH in Boston, Ani Patel with Tufts University. I do invite you to be part of the program. Give us a call, 800-433-8850. Send an email to drshow@wamu.org.
MS. DIANE REHMFollow us on Facebook or send us a tweet. And welcome to all of you.
DR. MARVIN MCMILLENWell, thank you very much.
MR. ANDREW SCHULMANThank you.
MR. JOHN POWELLThank you for having us.
MR. ANIRUDDH PATELThank you.
REHMAndrew, I'll start with you. You work as a musician in intensive care, units at two hospitals. Tell us exactly what you do.
SCHULMANOkay. I am a medical musician, which is a new term.
REHMI've never heard that before.
SCHULMANYeah. I started using that as a term a few months after I began playing as a volunteer at what was then called Beth Israel Medical Center in New York. It's now Mt. Sinai Beth Israel. I was part a visiting artist program of the music therapy department at the hospital and I had to come to a decision in the second or third month about really what I was going to call myself and what I was going to do.
SCHULMANI thought briefly about becoming a music therapist. I was very excited about that and then I went on the websites of several university programs in music therapy and saw that I'd have to go back to school for a couple of years. I was 58 years old at the time. And I was then and will always be a professional musician and I was only interested in one area of music and that is in critical care, working in an intensive care unit because...
REHMWhy?
SCHULMANMy life was saved in the Beth Israel surgical ICU by this gentleman here on my left and his team of great doctors and nurses. And so coming from that experience, having my life saved, I wanted to find a way to give back. And I asked Dr. McMillen if I could do so and he let me do that. And I just will briefly say that not only did he lead the team that saved my life and also give me permission to return to his intensive care unit, to me, even more important in that in my relationship with Marvin, is that for the last seven years, he's picked up the check at every breakfast, lunch and dinner we've had.
SCHULMANAnd for a professional musician in New York, that's a big thing.
REHMThat's a big thing. All right. Let's turn to Dr. McMillen. I know you're a trauma surgeon. Talk about how much music really does help in the trauma unit.
MCMILLENWell, there's three places that music has great impact. The article we always refer people to in The Lancet, a year ago, really showed the magnitude of what patient-selected music, mostly on their iPod, can do in terms of decreasing the need for pain medications and sedation. And from the point of view of cost, not only does that improve the patient experience, but it shortens the hospital stay. The second group -- the second place where music makes a difference and where Andrew has been so effective is there are many surgical patients who are going through an existential crisis.
MCMILLENAll of their support has been kicked out from under them. They are seeing the world with new eyes, struggling to get control of things. And to have a musician who is himself a recovered ICU patient who is very empathetic and very flexible and a great cabaret musician, can be a key element in their recovery. And finally, we have the patients we can't save for whom the family and patient are caught in the awful ritual of saying goodbye and the role that an empathetic musician can play in bringing them all together one last time to share something that is beautiful and make a connection to them can be enormous and they're very grateful and we do it for them.
REHMThat's a lovely thought. Ani Patel, as a psychology professor at Tufts University, you are also the author of "Music and the Brain." Does the research indicate that music has a real effect on physiology?
PATELYes, it does. And as Dr. McMillen was referring to, there are now more and more published studies showing this. Some involving giving music to patients undergoing surgery, showing that they will consume less anesthesia to achieve a certain level of sedation as measured by brain measurements, others showing better recovery post-stroke if they are involved in listening to music on a regular basis in a structure way compared to other sorts of treatments.
PATELMusic is not a replacement, obviously, for other treatments. It's a way of enhancing aspects of the healing process.
REHMAnd John Powell, you're the author of "Why You Love Music." Do you agree? You have a whole chapter in your book about music and medicine.
POWELLYes, indeed. One interesting way of looking at it is that our bodies are -- have sort of an internal pharmacy where they dispense various chemicals to us in various states. If you want to run away from a barking dog, then you need adrenalin and so on. And this pharmacy looks after you. And the interesting thing is that music has some control over what the pharmacy does and so if you are having trouble sleeping, it's probably because you got too much noradrenalin in your system and that increases your level of vigilance.
POWELLAnd if you want to reduce your level of vigilance, you can use classical music in the evening to calm down and you can tell the blood chemistry is changing and actually cure your insomnia, for example.
REHMConnie, is what Andrew does the same as music therapy?
MS. CONNIE TOMAINOThat's a good question. And it's similar in the way they -- it affects the patient's therapeutically. The field of music therapy and the term music therapy is the clinical and evidence-based use of music interventions by a board certified music therapist. And in the United States, the field of music therapy has been established since 1950 and there's always -- as Andrew mentioned, there's very rigorous academic training to become a music therapist not only under the graduate courses, but also graduate courses leading to a clinical internship of 1200 hours supervised and then a board-certified exam.
MS. CONNIE TOMAINOSo music therapists are really at the top of the clinical application of music in therapy. And I think what's happening and what we're seeing around the world is, with the emergence of good science by people like Ani Patel and (unintelligible) and other cognitive neuroscientists showing us the evidence of how and why music affects the brain, and wonderful and empathetic musicians like Andrew who are playing at bedside in the hospitals and insightful doctors like Dr. McMillen seeing the evidence of how this affects people in real time, what we're seeing is this need for collaboration of clinical music therapists, board-certified music therapists with the world of musicians who want to be a part of this evolution of providing therapeutic treatment in a very effective way.
REHMIndeed. And Connie, I know you, as a board-certified music therapist, you worked in coordination with Oliver Sachs.
TOMAINOThat's right. He and I started working together in 1980 and this was the facility where I still am, is his "Awakenings" facility, so his early experience with looking at music and rhythm specifically in making people who are frozen because of a Parkinson's type of disease come to life and be able to move with music are the patients that I started working with back then. And I've also worked collaboratively with him with people with Alzheimer's disease and especially in stroke rehabilitation.
REHMAnd how does music seem to work with stroke rehabilitation?
TOMAINOYeah. It's an important concept because what we've found in our research and also what the scientists are showing us now is that when we're using music, we're not just using the song, but we're using elements of music, rhythm and associations and emotions that are attached to that piece of music that are being processed in many areas of the brain. When somebody has a stroke, usually the stroke is localized with specific regions. But there's so many neural networks and pathways that get excited through that listening of music, that experience of that music, that we can actually stimulate, preserve pathways and preserve networks into action, action that that patient may not be able to produce on their own, but through a very prescriptive, directive use of sound and music and sort of jumpstart their brain into action again.
REHMConnie Tomaino, she's a board-certified music therapist. We'll take a short break and when we come back, hear more of Andrew's story.
REHMAnd welcome back. We're talking about the new uses of helping patients who are in stroke, in coma, in many other situations through the new use of music in intensive therapy in the trauma room. Andrew Schulman is with me. He is a musician who's written a book titled "Waking The Spirit: A Musician's Journey Healing Body, Mind and Soul." You actually began this work after you, yourself, were in a coma. Your wife played your favorite song. Tell us what happened.
SCHULMANWell, I had major surgery, and at the end of it, and it was a very lucky thing because I had a 99 percent diagnosis of pancreatic cancer, and in the surgery, if you get a 99 percent, somebody gets the one percent, and I did. It was incredible that it was not malignant. And the surgeon goes down to the waiting room and tells my wife this miracle, and they're jumping for joy, and his beeper goes off, get to the surgical ICU immediately.
SCHULMANAs they were wheeling me out of the operating room, I went into shock, and within a couple of minutes, I was clinically dead as they're racing me to the surgical intensive care unit. And they did resuscitate me, but I was put into a medically induced coma immediately, and over the next three days it was steady downhill. It was -- medicine reached its limit. My wife talking into my ear telling me she loved me reached its limit. Nothing was reaching me.
SCHULMANAnd then Wendy, my wife, had an epiphany that the only thing that could reach me was music, and the epiphany came because she saw my iPod in her bag, and she turned to the doctor, then Marvin was off-duty already.
REHMDr. McMillen.
SCHULMANYeah, it was Dr. Simon Iref, who was the attending then, and she said I think the only thing that can reach him is music, and he said, okay, try it for 30 minutes. And it just so happened that my ultimate favorite piece of music, the "St. Matthew Passion," was first on the list, and...
REHMAnd let's hear a clip of what your wife played for you.
REHMSo this is the "St. Matthew Passion" by Bach. What happened?
SCHULMANWell, the doctor had said 30 minutes only, and 30 minutes went by, and for the first time in three days I started to stabilize. I had been unstable every second for three days. And the -- by the -- all the medical things that had to happen started happening all of a sudden, including, amazingly enough, I had a terminal level of acid built up in my tissues, and it affected me on a metabolic level. Even the acid started to recede from the tissues.
REHMSo Dr. McMillen, what do you believe happened?
MCMILLENWell, Dr. Patel has written about how when we get chills to that little clip of "The St. Matthew Passion," that's a demonstration of the physiologic power that music can have, that literally our hair stands on end, we feel goosebumps. It's our nervous system responding to the music in a non-cognitive way. And as a classically trained physician I'm comfortable saying that playing familiar music would improve blood pressure and improve heart rate.
SCHULMANWhat's fascinating about what happened with Andrew and what I think physicians have to be open to is the idea he changed metabolically. Dr. Patel's lectures, which are quite wonderful, point how the functional MRI data is showing us that the -- there's so much more cortical activity with listening to music than just listening to speech. And could it be that the neuro-physiologic response to music is so great that it's even capable of affecting things at the cellular level? Because I've never seen this acidosis turn around.
REHMDr. Patel, do you want to comment?
PATELYes, one of the ideas that's emerging in studying music in the brain is that there's no single music center, that music engages wide areas of the brain and connects to many networks that we use for other regions like language, for example. It's been an area that I've worked on. But the great emotional power of music may be because it doesn't just activate one emotion system in the brain, it seems to activate almost every single emotion system at the same time in ways that very few other things can. And these perhaps are the reasons why we see these metabolic effects, as Dr. McMillen said, on basically physiology.
PATELSo it can affect things that are very low-level, almost innate responses to sound, all the way up to very high-level, culturally conditioned things that have to do with the associations that you have with a particular piece of music, like Andrew had powerful associations with "The St. Matthew Passion" that obviously played a role, I think, in his profound response to that piece.
REHMSo last year, Dr. McMillen, Lancet, the medical journal, released a paper concluding that music can aid in recovery after operations. Does that mean that you, as a trauma physician, should always have music playing in a trauma situation?
MCMILLENI used to know a heart surgeon who, in the routine part of the operation, would play Mozart, and then when he was sewing the heart grafts, would play Beethoven. He felt that the fine medical work required the Beethoven, the Mozart was too upbeat. And so this idea has been around for a while. I think we have to examine this in it many different applications and the role that it can play in the care of our patients.
MCMILLENI think the most important thing that Andrew and I have probably done and that I hope other -- we could help other groups build on, is we've become collaborators. I know more about music and the lift of a professional guitarist right now than probably anybody else in surgical critical care, and Andrew knows an awful lot about surgical critical illness, including the emotional state of the patient, the family, what ICU dementia is, what perioperative delirium is.
MCMILLENAnd so we have this ongoing conversation, now seven years into it, and we would like to see that expand, we would like to see other people learn from our failures and go on to develop their own areas.
REHMJohn Powell, you are both a physicist and a musician. Talk about how or why you think this area should be of growing interest to not only trauma surgeons but doctors everywhere?
POWELLYeah, the (unintelligible) is very interesting, and there have been lots of research which has shown recently that -- a few decades ago, people thought that music was localized in the brain to certain areas, but more recently they've discovered that music fires up connections all over the brain. So if the brain's slightly damaged in any way, then the music will make a contact anyway. So that makes it extremely useful because you can contact a person with a brain which isn't working properly through music, which is contacting all parts of the brain at once.
REHMBut let me ask you this. If the brain is receiving this music, and one is open to what music is doing for the brain, why wouldn't it work on other parts of the body if the brain is communicating that reception of music to the body?
POWELLWhen everything's working well in the body and the brain, then music does actually affect various parts of your body. There are various things we have very little control over. For example music, if you turn the rhythm of the music up or down, the tempo of the music, you can actually alter people's -- the speed at which they chew in a restaurant.
REHMThat's very interesting. I never thought of that. Andrew, in your book, "Waking the Spirit," you talk about several stories of patients who have been in comas or have been in trauma after surgery who responded to your Rolling Stones songs.
SCHULMANOh, I can actually use his name because he's given permission. It's Eliot Bernard, who is a very prominent businessman in England, and he had also a lifetime of not only loving music but being a very active part of the -- especially the classical music scene in England, the chairman of the board of several orchestras, et cetera. He had a major complication like I did at the end of a surgery and was really in terrible condition, and I had the experience of being able to go to him for about a week.
SCHULMANAnd it seemed it was helping him, but he was terribly ill, and then finally it was like the fourth day I came in, where I was asked immediately to go to the bedside because it looked like he was on the verge of permanent death. In medicine, there's clinical death, you can be resuscitated, permanent death, brain dead, and you're gone, really gone. And I had been told the day before by one of his close associates that he also loved -- he was a friend of Mick Jagger and loved the Rolling Stones, and I bought their full score of the Rolling Stones music and walked in, and I just intuitively went to that.
SCHULMANThe song I played for him was "Wild Horses." I just -- a lot going on with your intuition in these situations, and it has to be very, very fast because I thought of the line wild horses couldn't drag me away, and that's what I wanted him to hear. And this is a story I also put in the book and can tell because at that moment he was surrounded by doctors, nurses and his family. His face was completely placid and gray, as it looks like when you're on your way out, and within about a minute of that music, we could see it reach him because his brow started to furrow, and within another couple of minutes, fortunately "Wild Horses" is a long song, it's about a six-minute song, and I played it twice.
SCHULMANAnd by the end of the second song, all of a sudden the numbers -- when I'm sitting and playing, I'm watching the patient, the face, the hands and the feet, and every 15, 20 seconds, I'm looking at the computer monitor above the bed because I'm watching their vital signs. And we all saw it. And the brow started to furrow, and the numbers all of a sudden started to stabilize and change.
REHMInteresting.
SCHULMANYeah, and it basically did for him what "The St. Matthew Passion" did for me.
REHMYou have several songs that you play you call your penicillin pieces. Play that little "Theme in D" for us. You have your guitar with you.
SCHULMANOkay, yeah, yeah.
SCHULMANOops, sorry. One of things actually, guitars are notorious for quickly going out of tune. I'm very careful about the tuning at a bedside because even in a coma, people hear everything. And you have to have -- the sound and timbre and quality of the instrument makes a big difference. Okay, and being in tune. And I'm just going to say this is close enough for radio right now. Okay, here we go.
REHMAnd that was Andrew Schulman, professional classical guitarist and author of "Waking the Spirit," and you're listening to the Diane Rehm Show. And to you, Connie Tomaino, I gather there are studies to see if music therapy helps patients suffering from Parkinson's and dementia.
TOMAINOOh absolutely. There's been use of really fine clinical studies that I've done and colleagues have done looking at various aspects of music as treatment. For example with Parkinson's, the use of rhythm, just the beat and tempo of sound, similar to what John had mentioned before, that that can help organize and -- help organize gait as well as the initiation of movement in somebody in Parkinson's, and there's been some wonderful studies that show how precisely this rhythmic beat, this rhythmic auditory stimulation, can enable somebody with Parkinson's not only initiate movement but then carry over that movement while the rhythm is present.
TOMAINOSo we know for a fact that that works. There's been substantial research in that area, so much so that people with Parkinson's know that dancing and movement is one way for them to be as flexible as possible. With people with Alzheimer's disease, Ani had mentioned this before, and Dr. McMillen, as well, music of personal importance, when somebody loses their memory or ability to recall information, they don't really lose the essence of who they are or their totality of memory.
TOMAINOThe sensation, the associations, the recognition is still there on some level, and because of the lifelong associations we've attached to music of personal importance, similar to what happened with Andrew with the Bach piece, that excites so many aspects of brain function that somebody with Alzheimer's disease will recognize a familiar piece of music.
REHMInteresting.
TOMAINOAnd through that recognition come to in that moment. And the more we -- in our research that we show that the more we consistently use personalized preferred music, we're able to get that person not only to...
REHMAll right. We've got to take a very short break here. Your calls, comments when we come back.
REHMAnd as we talk about how music affects the human brain in sessions of trauma or recovery from stroke, here's a tweet from Ross, Dr. McMillen. Ross says, "Please talk about the anti-music that bombards patients in hospitals. The incessant alarms of the machines, etcetera."
MCMILLENThere's a wonderful organization in the United Kingdom, The King's Fund, which has studied the healing environment to -- in all aspects, architectural, music, horticulture, etcetera. The music part of it has been Live Music Now, which is Yehudi Menuhin's bequest. And he's absolutely right. I don't know what the optimal healing environment is, but I know it doesn't look like my intensive care unit.
MCMILLENAnd there's no need in an era of miniaturization and computerized things that can be broadcast, there's no need for it to look so bad. There's no need for it to be so intrusive. In fact, the response of people who work in ICUs to all those alarms going off, we often don't notice the respirator disconnect alarm, 'cause we're so used to it. And so the alarms are not achieving what we had hoped to.
MCMILLENAnd they're, you know, you don't sleep for an hour in an intensive care unit…
REHMI know.
MCMILLEN…at night. And we won't let our interns do that, but yet, every patient in our ICU is awakened every hour. And you don't get good sleep when you're sedated into sleep. You don't get the proper kind of REM sleep, which is a reprogramming. There's some of that in Andrew's book by a neuropsychiatrist named Steven Ullmann (sp?), who's really looked a lot at the actual role of sleep.
REHMSo you're really talking about a reorganization of the intensive care units. You're talking about the fact that you can do what needs to be done without the constant beeping, without the constant awakening?
MCMILLENWell, we've done a good job of bringing nurses, doctors, respiratory therapist and pharmacists together. I think it's time to bring in the musicians and the people who actually know something about the healing environment and look at what organizations like The King's Fund and Live Music Now have done before us.
REHMAnd John Powell, several studies have indicated that music can actually help reduce pain. Talk about that.
POWELLYes. It's quite interesting. Pain is not a thing. You can't measure it. If you stub your toe on a quiet Sunday morning, as you're walking around the garden, you might hurt it -- feel it very -- a lot. But if you stub your toe when trying to rescue a child from running into a road, you won't notice it. So it's not a standard thing. So it can be affected by how you feel and music can affect how you feel. So, of course, you can control pain, to some extent, by music. And they've actually done this in dental clinics, where they've given the patient the chance of choosing the music. And that works very well to reduce the pain, the perceived pain.
POWELLBut one of the best things they can do is to hand the patient the volume control. And they tell the patient, this volume control is a method of reducing your pain. And once they've been told that, they -- it really works very well.
REHMHuh. And Ani Patel, apparently there's some evidence that music could help alleviate the need for anesthesia during surgery.
PATELYes. There's a beautiful double blind placebo controlled study of that, treating music as you would treat a medication, where some patients were allowed to listen to music during a hip surgery for -- and others were given ocean sounds. So they also heard sounds that were supposed to mask the noises of the operating room. But the medical staff were not aware of what the patients were hearing. They weren't aware of the underlying hypothesis and so forth.
PATELAnd things were measured like the amount of anesthesia the patients required to reach target level of sedation, as measured by brain measures, the amount of stress hormones in their blood. And in both of these indices, the people that listened to music did better. They needed less anesthesia. They had lower stress hormone levels in their blood during the procedure.
PATELAnd if I can just add one other thing. A lot of what we've been talking about is the emotional effects of music. But I want to go back to something that Connie Tomaino mentioned about rhythm and Parkinson's and the interaction between the auditory and the motor systems. I think that's an important example of how the way music affects the body and the brain is more than just the emotion circuits. It affects other kinds of circuits. In this case, the motor circuits, and their intimate connection to the hearing circuits in people.
PATELAnd music can help us get to those circuits and it's kind of the fuel and the fire of neuroplasticity, that is the ability of the brain to change with experience. But the effects of music on the brain go beyond just emotion pathways.
REHMBut here's a question, a tweet, Ati (sic), does recorded music have the same beneficial effects as live music therapy?
PATELConnie, you want to take that one?
TOMAINOYeah, so recorded music, as we've heard, does have an immediate effect on people with Alzheimer's disease dementia, in people in post-surgical treatment as well. So again, recorded music that's of personal importance can have a great impact. The beauty of live, interactive music is that the music can be changed in the moment, in response to the actions or…
REHMInteresting.
TOMAINO…observed responses of the patient. So if they look like they're becoming more aware, the music therapist changing the dynamic of the music or adding a different rhythm to bring that patient more into that present experience.
REHMAnd for you, Andrew, of course, Beth Israel is a very diverse hospital. So you play Schubert, a Schubert piece for many of those.
SCHULMANYeah, this is something that really startled me when I first doing it. There's a famous serenade by Schubert. In German, it's "Standchen." And we have, as you said, very diverse in every way in terms of the patient population. And I found with this piece, to my surprise, that it just covered every demographic. And I tried figuring it out. And I have some ideas, but rather than tell you that, I'll just play some of the piece.
REHMGood.
SCHULMANI'll just play the opening of the piece.
REHMGood.
SCHULMANThat's not the opening. That's my tuning.
REHMAnd why do you think that piece appeals to so broad a universe?
SCHULMANWell, Schubert wrote this in the last months of his life. And so there is a very deep feeling of emotion in the piece to start with, that -- there's a little bit of a background, which I won't go into, what he was living with and what he was suffering with at the time. Also, this is in Vienna, which is a crossroads of the world at that time, between East and West. And you notice in the opening melody…
SCHULMAN…that these -- that there is -- it's Western music, it's Vienna, but it also has a scale pattern that connects to the East because in Beth Israel we live -- the hospital's near old New York Chinatown. And we have Chinese patients, who really don't connect to Western music. When I play for them, I will take a pentatonic scale …
SCHULMAN…which is -- Chinese music is based on it. I'll improvise and then they connect.
REHMInteresting.
SCHULMANBut on this piece, this is the one piece all of a sudden they did connect. Plus, there is something in this opening.
SCHULMANIf I change the rhythm and all of a sudden you're in pop city.
REHMExactly, exactly.
SCHULMANAnd so you -- and there are -- there's more to it than that, but this piece is one of the ultimate penicillin pieces I have. And it just covers everybody.
REHMJohn Powell, here's a tweet from another John, who says, "Is the Mozart Effect true or has it been disproven?"
POWELLWell, the interesting thing about the Mozart Effect is it's completely true and works very well, but it has nothing at all to do with Mozart. The original research was very interesting and published and fascinated everybody. Lots of school governors and even prison governors were playing classical music to people to make them more calm and bright. And it seemed to work. But basically a lot of psychologists then did a lot of research on the Mozart Effect.
POWELLAnd they found there was Schubert Effect, which is an identical. And then they found that if you read a short story to people you had an identical effect. Basically, if you give somebody something which is stimulating and that they enjoy, just before an I.Q. test, they'll do better in the I.Q. test because they're woken up, they're stimulated and also they're in a good mood.
REHMInteresting. All right. I want to go to the phones. Let's go to nurse Bob, in Naples, Fla. You're on the air.
BOBYes. And thank you very much, Diane.
REHMSure.
BOBKudos to your guests.
REHMThanks.
BOBYes, I played, well, over 400 times last year around Naples. And mostly memory units. And I see miracles every day. And as a nurse I've tried to do assessments while I'm playing and whatever it takes to get their attention I will. I'll take my foot and put it way up in the air, whatever. And when they start tracking me with their eyes, then I know I have them.
REHMAni, do you want to comment?
PATELYeah, that's an interesting observation. So you're using not just music, but every resource you have available to reach these patients. And I think the physicality, the movement, is really -- of course it's a deep connection that we have with music. We make music by moving. We move in response to music. And this deep connection between sound and movement is part of what makes music so powerful and it's being used in therapies, for example, to help people learn how to recoordinate their movements after a stroke by connecting the movements they make with sounds and using them -- those -- that relationship to help them tune and refine their patterns of movement.
REHMAnd you're listening to "The Diane Rehm Show." And to Janesville, Wis., Sid, you're on the air.
SIDWell, thank you, Diane, for allowing me to speak on your wonderful show.
REHMThank you.
SIDThis is a very important thing to me, music. I am an amateur musician. I play an accordion. And I play an accordion for hospice patients and dementia patients. And I play it in a very simple, tuneful way. And it's a very remarkable thing to do. I've found it extremely rewarding. And what I find is -- the nice thing is an accordion is a very versatile instrument. And some patients I have to play very gently to, something like "Take My Hand Precious Lord." And I play that in the right hand and a bassoon tone in the left hand with long soft drawn-out chords.
SIDAnd that is the thing they need. But then I had a fellow who was a skilled man, a laboring man all his life and to come across to him I played the "Beer Barrel Polka." And he was very excited to hear that.
REHMThat is just great. So this idea of using music, Dr. McMillen, in various settings, certainly your experience with Andrew has been in the trauma unit, but it sounds as though the effects of music for those who may have dementia, for those who are suffering pain, for those who have sleep disorders, may indeed have an impact.
MCMILLENYes. I really think there's a huge need right now for an educational foundation to take this on and become a catalyst for putting all of these various individuals together. I mean, we have some very specific lessons we've learned working with Andrew over the last few years. We did not have a great success rate with recorded music, unless it was patient designated recorded music. That made a difference. But just background music became Muzak.
MCMILLENAnd we would like to try to get everyone together once a year in the Berkshires. And we are hoping that we could get the Society of Critical Care Medicine to be more interested in the specifics of what we've done and learned. And this is -- this really needs lots of people working at individual parts. We haven't even touched on the possible role of vocal. I believe vocal might have -- vocal music might have great impact for suffering patients.
MCMILLENBut again, these are things we need to study and study requires focus and logistics. And clearly you've got five people on here who all care very much about this, but we gotta figure out some way of coming together and sharing what we know. And it's -- the important thing to realize is this stuff is cheap. By decreasing the need for pain and sedation in an ICU, you knock $3,000 in costs off the cost of that hospital stay. So, you know, a two-hour session where you've got music therapists or trained medical musicians coming into your ICU every day may actually have very, very substantial benefit, economically, from the hospital's perspective.
REHMAnd do you see that your professional colleagues are open to this idea?
MCMILLENI think it would surprise people how much surgeons worry about the patients whom we -- whose life we've saved, but who are not fully rehabilitated or whom we discharge to a nursing facility. And anything that would improve on that, we would embrace.
REHMDr. Marvin McMillen, trauma surgeon, Andrew Schulman, his book is titled, "Waking the Spirit," Connie Tomaino, a board-certified music therapist, John Powell, a physicist and musician, Ani Patel, psychology professor at Tufts, thank you all. Thanks for listening. I'm Diane Rehm.
After 52 years at WAMU, Diane Rehm says goodbye.
Diane takes the mic one last time at WAMU. She talks to Susan Page of USA Today about Trump’s first hundred days – and what they say about the next hundred.
Maryland Congressman Jamie Raskin was first elected to the House in 2016, just as Donald Trump ascended to the presidency for the first time. Since then, few Democrats have worked as…
Can the courts act as a check on the Trump administration’s power? CNN chief Supreme Court analyst Joan Biskupic on how the clash over deportations is testing the judiciary.