Diane’s farewell message
After 52 years at WAMU, Diane Rehm says goodbye.
Guest Host: Nia-Malika Henderson
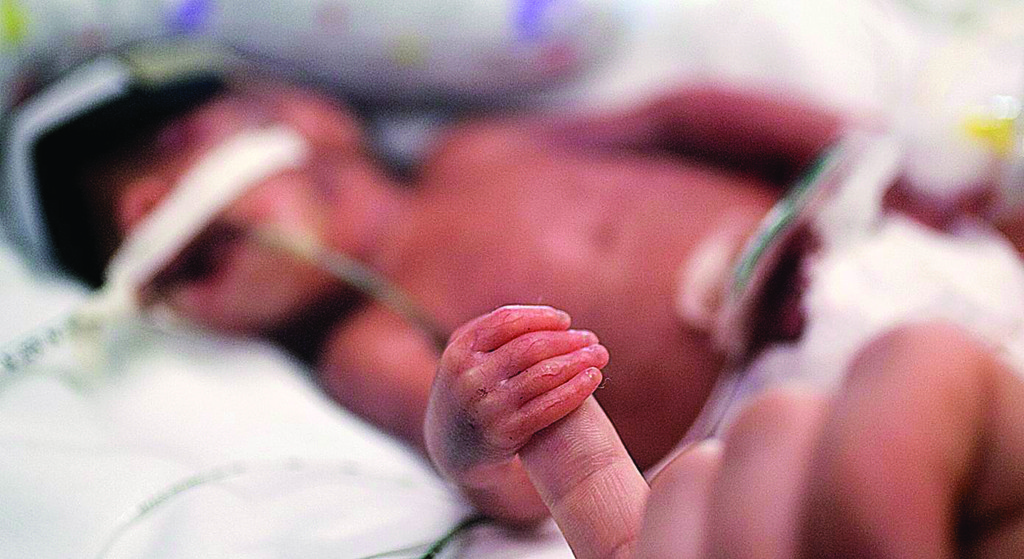
Juniper French was born at 23 weeks, weighing just over a pound.
Juniper French was born four months early, at 23 weeks’ gestation. She weighed just over one pound. She was on the edge of viability — a so-called “micro-preemie.” Several decades ago, she never would have survived. In order to live, she would be constantly hooked up to machines and monitors. If she survives, she might be severely brain damaged. Juniper’s parents — journalists Kelley Benham French and Thomas French — had to decide what they were willing to do to save her or if the greater act of love was to let her go. Guest host Nia-Malika Henderson talks to them about navigating what is medically possible and what is right.
Reprinted with permission.
Juniper: The Girl Who Was Born Too Soon by wamu885 on Scribd
MS. NIA-MALIKA HENDERSONThanks for joining us. I'm Nia-Malika Henderson with CNN sitting in for Diane Rehm. Juniper French was born four months early, weighing just one pound four ounces. In a new book, Juniper's parents describe, in painful detail, what it's like to spend months in limbo caring for a micro-preemie in the hospital. The title of the book is "Juniper: The Girl Who Was Born Too Soon." Authors Kelley Benham French and Thomas French join me from WFIU in Bloomington, Indiana.
MS. NIA-MALIKA HENDERSONAlso, we'll be taking your comments, questions throughout the hour. You can call us on 800-433-8850. You can also send us an email at drshow@wamu.org. You can also join us on Facebook or on Twitter. Thanks so much for being with us today, Thomas and...
MR. THOMAS FRENCHThanks for having us.
HENDERSON...and Kelley. I want to go directly to this. You guys are both reporters. And the book you wrote, a very personal book, tell us how this book came about. Kelley?
MS. KELLEY BENHAM FRENCHWell, when Juniper was in the hospital, there was no time to think about a book. It would've just been crazy. But when she came home, I guess I had two motivations. One, as her mother, you know, to capture this for her so that she knew what she had been through and how strong she was and who had loved her and how hard she had fought. And then, as journalists, I felt a real responsibility to tell this story because it's right at the frontier of medicine and the healthcare debate and so many huge issues and enormous questions.
MS. KELLEY BENHAM FRENCHAnd we had this incredible access to this really kind of sacred thing.
HENDERSONAnd Thomas, you take turns writing the different chapters in this book. And how -- tell me about that experience. It was, apparently, your idea to write the book.
FRENCHWell, I had to figure out a way that we could both write it without trying to speak in one voice throughout because to go through this experience, you are together, but you experience it very separately, both due to your biology and to our different sensibilities. And it just seemed like it was the only way to tell the story. We couldn't really do it with just one or the other. We needed both voices.
HENDERSONAnd Kelley, even before Juniper, you were experiencing fertility problems.
FRENCHRight. It took us four and a half years to get Juniper. It took many rounds of IVF, all of our savings, all of our patience and ultimately an egg donor.
HENDERSONAnd once you got pregnant, there were some -- there's that accidents that happen, some problems.
FRENCHI actually had like a -- just a perfect, perfect pregnancy. The doctors really struggled to figure out what could've caused this. The only thing we could come up with was, like, a very minor bike accident a week or two before I went into labor. And then, actually, the day I went into labor, my dog, just being exuberant and playful, jumped up and kind of smacked me in the belly with her head. That's the best we could come up with, but you know, pregnant women are tough.
FRENCHPregnant women carry kicking toddlers around. They trip and fall down stairs and don't go through what I went through so I can't really say for sure what caused it.
FRENCHYou know, it was one of those things where she had this really smooth pregnancy up until that exact moment when she didn't. And a lot of the story is about you're going along, you're just -- you think you're going to have a baby and then, suddenly, out of nowhere on a day you least expect it, you're rushing to the hospital.
HENDERSONAnd as the doctors tried to delay the labor, they asked you to decide whether or not to make every effort to save her.
FRENCHOh, my goodness. This neonatologist visited us the day before she was ultimately born and he was a nice man and, clearly, a compassionate and good doctor. And he just started reciting this litany of disability and he said, you know, we can try to save your baby. Our baby was born at 23 weeks gestation, which is right at the border of viability outside the womb. You know, most people think of it loosely as around 24 weeks and we had been told, you must make it to 24 weeks or you might as well deliver your baby at home.
FRENCHAnd she came at 23 weeks and six days. So this doctor said, we can try to save her, but that might not be what you want because in a premature baby, a baby that unfinished, every system in their body is underdeveloped and there's no way for them to predict what might happen to the brain, to the heart, to the lungs, to the gut. She could be damaged really to any degree in any part of her body or her mind.
FRENCHThe doctor was very nice and very calm, but there was something about his calm, which in that moment, I had this very emotional reaction. I wanted to punch him because what I heard him saying, even though he didn't say these words, was that he wanted us to kill our baby.
FRENCHThat's totally not what he said, but...
FRENCHBut that's how it felt, because he was basically telling us, you have to think about whether this might not be selfish of you and your husband to actually fight to save her because she may end up with a life that she ends up being angry with you and resenting you for the rest of her life if you -- if things go wrong. So it was just -- it was a very emotional moment and there was something about that calm and the lack of better information.
FRENCHWe desperately searched online for any kind of information that would help us make this choice of whether or not to let them try to save her or not. And what we found was that you can easily find better information on how to pick out a toaster than on how to make this decision.
HENDERSONWow. And I wonder, if you could, Tom, read -- first of all, this book is beautifully written. You guys are such great writers and just sharing your story in such a personal, revelatory way. I wonder if we can turn to page 91 and begin with you, first, Tom, and set up what's going on here.
FRENCHSure. This is right at 23 weeks, six days and Kelley is in labor, but the nurse doesn't believe her, thinks that she's having constipation pains and the nurse isn't believing her and Kelley's actually about to give birth, so. Excuse me. "Something is wrong, Kelley said. I know something is wrong. The next contraction was coming. Her grip tightened on my hand. Soon, her eyes were closing and her mouth was widening into an O and her face was growing more and more rigid until it shattered with her cries.
FRENCHDuring a lull between the spasms, I ran out to the nurse's station and told her to get a doctor right away. Eventually, a young resident arrived and snapped a glove onto his hand to check her cervix. She was sobbing now and gulping for air and she asked him not to do anything that would hurt the baby. He told her to be still and breathe. Please be careful, Kelley said. Please be careful.
FRENCHThe room was dark, but when the resident stood up, enough light poured in from the hall that I could see the startled look on his face. Another resident materialized, someone more senior, and when she checked Kelley, a look came over her fact, too. We have to get you to an operating room, she said. 24 weeks, they had told us the baby had no chance unless we made it to 24 weeks. We were now at 23 weeks and six days. Kelley begged the doctor to do something, anything to delay the delivery.
FRENCHThe doctor shook her head. The bag is coming out, she said. I could feel two feet kicking."
HENDERSONWow.
FRENCH"It destroyed me, seeing Kelley scrabble for more time. Better than anyone I knew the ferocity of this woman's will to be a mother, but I had never seen it expressed with such desperation. I’m sorry, sweetie, the doctor said. We have to go now." At the double doors leading to the OR, they told me to wait. I paced back and forth and thought about my sons, Nat and Sam, unaware that their little sister was crashing her way into the world.
FRENCHI wondered if she could -- would live long enough for them to meet her, if she would have the chance to look in their faces and hear their voices. The thought made me gasp. A nurse came out and handed me scrubs. She told me I would be with my wife shortly. The doors opened and the nurse motioned me back. I saw Kelley stretched out on the table, the doctors gathered around her in their blue masks, the bright light beaming a circle of pure white onto her belly.
FRENCHA roaring filled my ears, a rushing sound like a mad wind. This is what it must be like, I told myself, to jump out of a plane."
HENDERSONAnd you, of course, Kelley, have a very different perspective on this. Your husband is there watching you being wheeled away and you are there being wheeled away. And when we come back from break, I want you to read as well. But I want you to talk about how you were feeling in that moment.
FRENCHOh, it was terrifying. That's so simplistic to say that I was terrified, but I was terrified. I thought after everything we had done to bring this child into the world, she was going to be born and live just long enough for us to watch her die.
HENDERSONWow. And I wonder, for other parents, I mean, who are dealing with this, what kind of message do you have for them? I mean, 'cause you had to make a real choice there and it sounds like Tom was Googling information. And what would you say to other parents in this situation?
FRENCHWell, stay off Google. Google's not helpful. And the reason it's not helpful or interesting, there are a lot of statistics on Google, but many of them are outdated. It doesn't take long in neonatology for statistics to get old and become irrelevant. A lot of the statistics are also from other countries that don't have the tradition of intervention and aren't as good at saving babies as we are here. So there's actually a lot more hope than is available on Google.
HENDERSONComing up, more of our conversation about "Juniper: The Girl Who Was Born Too Soon" with Kelley and Thomas French.
HENDERSONWelcome back. I'm Nia-Malika Henderson with CNN, sitting in for Diane Rehm. Joining me today, Kelley and Thomas French, who have written about their daughter Juniper in a book called "The Girl Who was Born Too Soon." Kelley, I want to go right to you, and read, if you will, from your book, starting on Page 93, if you could, and set this scene up. And this is the corollary, of course, to Thomas, who was watching you being wheeled away.
FRENCHSo now we're in the operating room. I heard voices. The doctors were talking about a movie they had seen. I wanted to yell at them to focus because didn't they realize that a half-formed human was being ripped from my body and that she might only have right now, these few minutes or hours, and wasn't that enough to get their attention. But I couldn't yell. I held Tom's hand. I turned my head toward him and threw up.
FRENCHI could see the giant, round light above us, a hovering spaceship. I felt a sickening tug. I knew that we were two separate people now. She's kicking, Tom said. He was peering over the surgical drape at the gaping red meat of my abdomen and at the unfinished child that had just emerged from it. Someone said she cried, but I didn't hear it. I tasted prune vomit in my mouth.
FRENCHSomeone slipped a piece of paper in front of me and an inkpad and asked for a fingerprint. On the paper were two still-wet footprints, each an inch and a half long, startling evidence that she was here. She weight 570 grams, one pound, four ounces. She was 11 and a half inches long, the length of a Barbie doll. My baby, I kept saying, my baby, my baby.
FRENCHI saw the nurse roll the incubator past. Inside was a raw, dark blur in a too-big hat. Tom looked at me and looked at the baby. Go with her, I said, please go.
HENDERSONAnd Kelley, your daughter Juniper, at this point she weighs just over a pound. You say she is the length of a Barbie doll. And the doctors, you decide you want the doctors to save her, but the risks involved and the procedures are great in terms of what the outcome might be.
FRENCHSo every treatment exacts some -- some cost. And what -- what helped us make the decision was a conversation we had with another nurse, who just said, you know, it's a process. You don't have to decide all in one moment. You can let her be born, we can evaluate her. Some babies might come out blue and limp, and some come out pink and crying, and in the first few days, we'll learn a lot. We'll learn whether she has bleeding in her brain or any other serious insults as the result of her birth.
FRENCHAnd there's a window of time in the first few days or weeks when if it looks like she is not going to have a good quality of life, we can reverse course and take her off life support. So the choice that we made really was to give her a chance.
HENDERSONAnd you both learned how to navigate the NICU and the heart and the lung monitors and the oxygen levels. Thomas, can you talk about that experience, which I imagine must have been so overwhelming, as neither of you are doctors?
FRENCHWe're not doctors, and we don't even play doctors on TV. Yeah, it was completely bewildering, you know, all the language that they used, the acronyms that they used at morning rounds, all the monitor readings, all the beeping and the alarms. And at first you just -- you just sort of get washed away in it, and you flow with it as best you can and hang on as best you can.
FRENCHBut as the days went on, I started to learn, and Kelley of course started to learn, what some of those acronyms meant and what the doctors were -- exactly what they were saying and what -- what it meant, what was showing on the monitors. And what was hard was that sometimes, once we understood them better, it was all the more terrifying because what they were saying for those first weeks and into months was really hard.
HENDERSONAnd I wonder, we're getting a lot of emails on this one, and this is an email from John, and Kelley, if you want to take this, this is about the doctors, and he wonders, he says, there are so many medical issues you were faced with, do you think you need your own special doctor to advise you rather than deal with the doctors who were often negative, giving you the voice of doom?
FRENCHI think the more support families can have in that moment the better. Yes, what's interesting is you don't have one doctor. You have a rotating team of neonatologists and specialists and nurses and nurse practitioners and therapists, and they all bring different perspectives to these questions. And -- it's John, right? Doctors -- studies do show that doctors tend to be too pessimistic when they try to forecast outcomes for very, very early babies.
FRENCHAnd there are a lot of reasons for that, but what would have helped me, I think, would have been access to other parents who had been through this, who had had a range, maybe, of different outcomes and also some of the research that showed how much power parents actually have because you feel so helpless. You feel like all you can do is sit by incubator and cry, but that's not true at all, and the studies show that the biggest advantage a baby can have is an involved family.
HENDERSONWe have an email from Virginia here. She says, thank you to Juniper French's parents and to "The Diane Rehm Show" for showcasing this story. As the mother of a toddler born as a 28-week-old preemie, it's reassuring to hear about stories like this, which get little exposure. It's a very trying experience that many should know more about. I wonder -- one of the things you talked about in terms of the care, and there's a team of doctors and a team of nurses, but you guys also chose a certain nurse to be Juniper's primary caretaker. Thomas, do you want to talk about that?
FRENCHYes, it helps to have a primary nurse on the day shift and another one on the night shift, and we first figured out that the nurse we wanted for our primary on the day shift was Tracy Hullett. Tracy was the nurse -- I mean, there's a lot of terrific nurses on that floor, but Tracy was the nurse who other nurses were going to, to ask for advice on handle different issues with babies. And she just obviously knew what she was doing at a level that was very inspiring.
FRENCHSo it's true that we picked Tracy, but then Tracy had to decide whether she wanted to say yes because it's a tremendous emotional commitment to decide she's going to fight and give it her all for this baby because a lot of times these babies don't make it. The doctors are pessimistic, sometimes because they have seen some outcomes that are very sad.
FRENCHWe watched babies dying within a few feet of us during our stay there, and so we knew that death was not theoretical in this place. And Tracy we thought was our best chance, one of our best chances, at trying to give our daughter an edge. And so Tracy had to decide for herself whether she wanted to make that leap of faith, and ultimately she did, and I've got to say that Tracy saved our daughter's life more times than we can count. She was terrific, and she's still a good friend and still keeps in touch with Juniper, and we just -- we're very, very thankful and grateful to her and the rest of that medical team.
HENDERSONAnd you, Kelley, on -- in a section here on Page 124, you talk about how tiny your daughter is. When she's born she weighs about 570 grams. I wonder if you could read this single page, Page 124, when you write about your daughter's weight.
FRENCHSure. Things that weigh 570 grams, one, a six-week-old kitten, two, a Smith and Wesson Lady Smith double-action .38 special revolver, three, a bottle of Gatorade, four, a raw, bone-in ribeye, five, the left lung of an adult human female, six, the amount of breast milk an eight-pound baby drinks in one day, seven, $2.28 in pennies, eight, an adult eastern gray squirrel.
HENDERSONAnd Tom, you also write about this, your daughter's weight, how tiny she is.
FRENCHYeah, one second, Kelley closed the page. Excuse me. We sought escape wherever we could, the hospital cafeteria, the sixth-floor lounge, where we watched old episodes of "Law & Order." Once afternoon I went to Publix just so I could remember what it was like to push a grocery cart. I was in the produce section hunting for a decent bag of green grapes when I heard the alarm from the baby's monitor, warning that her oxygen saturation was dropping.
FRENCHI looked up to check the (unintelligible) number and was starting to wonder where the nurse had gone when I realized that the only thing above me were fluorescent lights. The alarm stopped. Seconds later, it started again. This time I ignored it until I could hear were the wheels jangling across the linoleum. I pushed on, trying not to think about the hospital, but when I came to the baking aisle, my hand reached for a small bag of sugar.
FRENCHI placed it in my palm, lifting it up and done, gauging the lightness of it. One pound was nothing. One pound could be poured away in an instant. The other shoppers pushed their carts around me, pretending they did not see the strange man crying over the sugar.
HENDERSONWow, and you both write about the importance of holding preemies skin to skin, and Kelley, could you talk about that, why that's so important and how they benefit Juniper as she's progressing?
FRENCHAbsolutely. NICUs around the world are starting to realize that allowing the mothers to hold the babies is not just a sweet and compassionate act, but babies clinically do better when they're with their moms. They breathe better, they have higher oxygen concentrations in their blood, and they just turn out better when they spend time skin to skin with their moms.
FRENCHSo NICUs are doing all kinds of things to include families in the care of these infants from the first day, and one of the most important things that our nurse -- our nurses did was they pulled us in because the babies are so terrifying, you can want to run, and some families do. But Tracy said put your hands in here and change her diaper. Reach in. This is your daughter. She would put little bows on her. And all of those tiny acts just helped us connect with her, and that was really crucial.
FRENCHIt was tough at first. Tracy wanted to put her in some clothes, but there were no clothes small enough, even clothes that are made for micro-preemies, so Tracy went to a dog store and bought clothes for a Chihuahua and put them on our daughter.
FRENCHAnd as it turns out, Chihuahuas dress pretty well. They're pretty fancy dressers.
FRENCHThey are.
FRENCHSo she had some pretty -- Juniper had some pretty crazy get-ups in that incubator. But that was her -- one of Tracy's ways of getting us to connect. Another thing that we realized, and we learned later on -- had heard it put really well by Jad Abumrad on Radiolab, was that sound is a form of touch, and for -- for the first couple months, I could not -- was not allowed to hold Juniper, but I was really desperate to reach her.
FRENCHAnd so one of the things I started doing was sitting beside the incubator and reading to her every day not because she was going to understand what I was reading, I was reading actually from Harry Potter, which is a very important book to -- in our family, but because -- I knew she wouldn't understand what a wizard was or a witch or a broomstick, but I wanted her to hear my voice, and I wanted her to hear the rhythms of those senses and a sense of something unfolding that was worth waiting for.
FRENCHI asked Tom, like, maybe "Goodnight Moon" would be a better choice, and he said, no, he said a story is a promise that the end is worth waiting for. So he read her a book about -- where children can fly and where a baby is saved from the most terrible evil in the world because his mother stood beside him and protected him with her life.
HENDERSONSo she would have something to look forward to. I'm Nia-Malika Henderson with CNN. You're listening to the Diane Rehm Show. If you'd like to join us, call 1-800-433-8850. Or send an email to drshow@wamu.org. You can also find us on Facebook or send us a tweet. We're getting a lot of emails here, and one of the things people want to know about is the cost of this. Tony from Washington, D.C., says my son was one pound, 12 ounces at birth in 1993. He's now 23 years old and in graduate school. There's hope at the end of the tunnel. Please talk about the importance of insurance.
FRENCHOh my goodness, shout-out to Blue Cross Blue Shield. Cost is one of the questions that I think people are sometimes afraid to ask. I'll just -- I researched it. Our baby's care cost $2.4 million, of which the hospital collected a negotiated rate of $1.2 million. We had fantastic insurance from Blue Cross Blue Shield. So her hospital stay cost us 400 bucks.
FRENCHIf she hadn't -- if we hadn't had that insurance, Medicare or Medicaid, I always get them confused when I'm stressed out, would've taken care of is, but what I learned as a journalist as I was researching this, because friends would ask me, hey, wouldn't it be better if we should -- if we vaccinated a million kids in Africa than spend so much on one small baby? And I didn't know. So I just said, well, better for who.
FRENCHBut in reporting it out, what I discovered is that actually dollars spent in the NICU are some of the -- that's some of the best bargains in medicine because those dollars buy so many years of useful life, and when it's compared to what we spend on the very, very old and sick, it's pennies.
HENDERSONThis process was also not only costly, but it was obviously very stressful, and it put a strain on your marriage. Tom, could you talk about that?
FRENCHSure. You know, when we went in, I had this idea in my head that Kelley and I were going to stand valiantly together by the incubator and buoy each other up through this -- this ordeal, and we were going to really help each other and be stronger together. And we -- those things did happen. We did buoy each other up. But it was a lot more complicated than that. There were times when the grief or the sadness you're feeling, the sense of absolute terror, it was also harrowing sometimes that one or the other of us would just sort of retreat inside ourselves and just kind of curl up.
FRENCHAnd there was a -- there was a period there toward the beginning when it was really hard for us to reach each other because I think we were just struggling to get through day by day and make it -- well actually hour by hour. We were told that -- we were -- you know, it was really made clear to us that we might go down to the hospital cafeteria to get lunch, and Juniper might be gone by the time we got back because these babies can, you know, can fade so quickly.
FRENCHSo living with that much stress isolated us for a while, but eventually we found our way through that, and I think we did come together much more as the months went by.
HENDERSONComing up, your calls and questions for Kelley and Thomas French, who have written a book, "Juniper: The Girl Who Was Born Too Soon."
HENDERSONWelcome back. I'm Nia-Malika Henderson with CNN, sitting in for Diane Rehm. With me today, Kelley and Thomas French, who's written a book, "Juniper," about their daughter, "The Girl Who Was Born Too Soon." We're gonna go now to a caller. Denise in Charlotte, N.C., you're on the air with "The Diane Rehm Show."
DENISEGood morning. Thanks so much for allowing me to join you today.
HENDERSONThanks for being here. What's your question?
DENISEIt's not so much a question as it's a statement and an inquiry. First I want to thank you guests. The topic is fantastic. I am a mother who had a preemie born at 27 weeks. She is now 15 years old and she's doing fabulously. But everything that's being spoken about is so important. And what I was wondering was if the discussions your guests have had with NICUs currently and today, are they doing anything to help those new parents while they're freshly experiencing the trauma?
DENISEBecause I remember feeling so alone, even though I was surrounded by four other preemie babies, we were all kept so insulated from one another. Maybe it's for HIPAA rules, I don't know. But is there a movement to help parents cope together? Because it's unbelievably trying on the new parents. And I can take my answer off.
HENDERSONThank you, Denise. Kelley?
FRENCHThat's a fantastic point. And if there's a movement, I'm not aware of it. Maybe Diane (sic) and I should start one. But what I have found is a lot of groups on social media that are incredibly helpful, like "Micro-Preemie Moms," support groups and things like that. But I do think that hospitals concern with HIPAA and with privacy laws makes it very hard for parents to connect sometimes in the hospital.
FRENCHOne thing that was really interesting was that it was overwhelming, but I didn't feel alone. We had terrific friends and family, colleagues, we had tremendous amount of support, which we were very, very fortunate for. And the doctors and nurses, I mean, honestly they were unbelievably wonderful. And, you now, Dr. Jermaine (sp?), who was the one I wanted to punch that first day when he gave us this bad news, I realized later that that was an emotional reaction and he was working really hard to save our baby.
FRENCHAnd in fact, there were some crucial points in the months that followed where Juniper's life was on the line and Dr. Jermaine was there in the middle of the night fighting really hard. And gosh, I looked back on that moment where I wanted to throttle him and I just felt bad. But, you know, he's a very understanding guy. And there were so many doctors and so many nurses on that floor who just gave their all. Kelley makes the point in the book that, you know, there was this incredible technology helping Juniper survive, but every single time she reached a crisis, the real difference was made by the human beings on that team.
HENDERSONAnd you guys also write about the history of caring for preemies. The uglier side of that, and sometimes in the past it had been racist and sometimes exhibitionist in terms of dealing with preemies.
FRENCHYes. During the teens and '20s there was, as the eugenics movement took hold, there was a lot of argument from doctors and other help experts around the country, basically talking about calling these babies weaklings and suggesting that they should be simply allowed to die because they were a problem for the country's genetic pool. Many of these babies were immigrant babies or minority -- babies from minority families.
FRENCHAnd there was a definite racist, xenophobic undertone to this rhetoric. Which, you know, joined with the rhetoric of the Nazis not long after that. But the exhibitionist side of it is one of the early doctors who really made a serious contribution in neonatology, even before it was called neonatology, was Martin Couney, who was a doctor from Europe who began -- after doing some exhibitions in Berlin and London, and possibly Paris, if my memory serves, he came over to the U.S. and began treating preemie babies in little wards or units that he would set up at World's Fairs or at Coney Island.
FRENCHAnd he would charge admission for people to come and see these babies. Now, that sounds kind of cruel, but honestly he used that admission to cover the very high overhead of taking care of these babies. And these parents and the babies who survived, who came back to see him, were all really grateful for what he had done. And it was kind of a trade-off. You know, putting the babies on display for people's curiosity for saving their lives.
HENDERSONI'm gonna go to another caller here. Mark, from Katy, Texas, you're on the air with "The Diane Rehm Show."
MARKIt's Katy, Texas, but that's fine.
HENDERSONKaty, Texas.
MARKThat's fine. Yeah, it's a wonderful story. Not to make light of it, but the nine out of ten situations like this that turn out badly they did not write a book. And they're not calling into the show. And so we want to keep things in perspective here. And also, she already made the point about the tremendous cost of these babies. And somebody bears the cost. And I'm sure that it's gonna have an effect on the future rates of Blue Cross Blue Shield.
MARKAnd, you know, I don't think that this level of care at the beginning of life -- and she mentioned the tremendous cost at the end of life, which has even less payback. We wouldn't have that if the system wasn't set up to generate profit. It's a for-profit system. And if it will save your life one day, but cost a million dollars, they'll do it if they can make some profit. And I'll take my response off the air.
HENDERSONAnd Kelley, you want to take this?
FRENCHLet me take that one. Yeah, that's a reaction we get a lot. And it's just untrue. It's just not based in fact. Mark mentioned nine out of ten babies that don't have this outcome. Well, it's not actually nine out of ten. What we learned as we looked into the research more and more is that even a baby as early as Juniper, which is absolutely the earliest that a baby can even have a prayer of being saved, if they live, the odds that they go on to have a great life with -- and be totally normal and go to school and join the cheerleading team are about half.
FRENCHThose are odds that I would take in a heartbeat. The research is just actually pretty optimistic. You know, doctors get a pessimistic view of it because they see kids when they're discharged. And when they do studies they say a baby has had X number of morbidities by discharge. Well, by their measurement Juniper had five of the serious morbidities, which is a disability that a very premature baby can have. But all of those resolved by the time she got home. She came home on no medicine, no monitors, no machines of any kind.
FRENCHAnd I don't think anybody could look at this little girl who is at kindergarten right now and call her an unfavorable outcome. So those statistics are -- that's just not real. That's not what they are. And then with the cost, I mean, I've explained it already. Insurance companies are happy to pay for very premature babies like Juniper because those are the best dollars they spend. They buy the most years of good life.
HENDERSONAnd Juniper finally came home 196 days after she was born. Thomas, tell me about that day.
FRENCHThat was both a wonderful day and a terrifying day. We had grown so accustomed to Tracy and the doctors and the other nurses helping us learn how to do everything, that it was a little bit terrifying, this idea that we were gonna take her home and she was gonna be off all the monitors and all the machines. And Tracy wasn't gonna be at our side. And we were gonna be on our own.
FRENCHSo that was very scary. But Tracy, who walked us out to the car and was crying and hugging us along with everyone else, she told us that when we got Juniper home she would instantly take a huge leap forward in there development. She would blossom. Because as hard as we'd worked reading her "Harry Potter," singing to her Springsteen songs, as hard as we worked to make that room entertaining and interesting and stimulating for her, it was still just a dark hospital room.
FRENCHAnd so we got her home and I can remember we laid her in her little seat, her little baby holder on the carpet in her room. And she just lit up seeing all the colors of her room and the sunlight pouring through the windows and it was a remarkable day.
HENDERSONAnd did either of you have any qualms about writing in such detail about her early years? Any concerns about her privacy going forward?
FRENCHGod, yes. I had a lot of concerns about it. It's not -- I'm not a real public person, actually. Tom is the sharer in the family, I think. I hadn't even posted that I was pregnant on Facebook or anything like that. And a lot of the people who are -- my close family members, many of them found out that Juniper was conceived with IVF and an egg donor when they read it in the newspaper. 'Cause I did a series before I wrote the book.
FRENCHBut ultimately what I decided is that, you know, she is a baby in the span covered by this book. I would feel very different, I think, if I were writing about her middle school years. She is the center of the book, it's about her to some degree, but it's more about these larger questions and it's much more revealing about Tom and I than about anything about her, other than just her incredible will.
HENDERSONAnd she knows about the book.
FRENCHOh, gosh, she says, "Mommy, take me to Barnes and Noble so I can see my butt on the cover."
HENDERSONOh, that's fantastic. And obviously she's doing well now. You mentioned she's in kindergarten. What -- how is she coming along?
FRENCHShe just started in kindergarten. We're really excited. She's in a great school with a wonderful teacher and really sweet families all around her and kids around her. She's got some fine motor skills that she's still working to catch up on. She's a little bit shy sometimes. But that usually lasts about 30 seconds and then she's -- then she really opens up. So she's doing really well. We were worried about, you know, would it affect her to have a book with her foot on the cover and her name to the book coming out.
FRENCHAnd we asked -- Kelley asked her kindergarten teacher who told her that, you know, honestly this is a good point in her development because you can't make a five-year-old anymore narcissistic than they already are naturally. So we, yeah.
FRENCHWell, yeah, we just -- our -- sort of our journalistic integrity require that we put everything in, which was tough sometimes because it's not always a tremendously flattering portrait of us.
HENDERSONRight.
FRENCHYou know, we were tired and stressed out and that was the harder part, I think, was our vulnerabilities.
HENDERSONI'm Nia-Malika Henderson with CNN. You're listening to "The Diane Rehm Show." So speaking of this being a difficult time in your marriage and just such a stressful thing, we have James who is from New Boston, Texas, and he has a question.
JAMESHi, y'all. I myself went through a dramatic experience when my daughter was born three years ago. I actually almost lost both my wife and my daughter at the time. And ironically, my wife wants to have another baby. And her and I have been discussing this. But I basically, I have a real issue with it 'cause I'm -- I myself still have not even recovered from the traumatic experience when my daughter was born. And I mean, my question is how long have y'all -- did it take y'all to basically recover from the traumatic experience?
FRENCHThere's still triggers sometimes. Sometimes I'll be holding her at night, she'll drift off beside me and I'll just start to cry watching her breathe. But what I did is I -- when I decided to write the book, I got pretty serious about getting some therapy with someone who specializes in trauma. And I did some things that were developed for soldiers with PTSD. And I did that because I wanted to keep the writing of the book separate from my person issues. I didn't want to be working out my trauma on the page. I wanted the book to stand on its own. And, you know, it's written for a mass audience. I didn't want it to sound like the diary of a, you know, of a crying mom.
HENDERSONI want to go now to Susan from Potomac, Md. Susan, you are on the air with "The Diane Rehm Show."
SUSANHi. Yes, thank you so much for taking my call. I am, too -- my husband and I had a son born at 23 weeks gestation. He was one pound, five ounces. And when you were trying to put that into an image, he fit into my -- the palm of our hands. Not that we could hold him, because it took another 30 days until the first time I could hold him. And he was in the NICU for, oh, for 108 days. He come home at five pounds, eight ounces. And that was 16 years ago.
SUSANAnd what you were sharing with us, was exactly how we dealt with it. The fear, the hope, and every day was different. You didn't know what would happen when you went into the NICU, what tube was where, more tubes placed in him. So I just wanted to say thank you because I'm shaking with my feelings right now. So…
FRENCHThank you, Susan.
FRENCHSo glad your son is okay. One thing that, you know, we learned slowly during those months in the NICU was that we had no idea if Juniper was gonna make it out of there, if we were ever gonna be able to leave the unit holding her. But we realized at a certain point that she was alive right now. She was alive right in front of us. And whatever we did, whether we had another day with her or another 25 years with her, we needed to make that day as good for her as we could. We wanted her to have a good day every day and for us to appreciate every day that we had her.
FRENCHAnd that was a really important realization for us and really helped us. Once we understood that it wasn't so much that we couldn't really think about what was gonna happen 10 years from then, we had to think about, look at this baby right in front of us, right in that moment and do our best to love her.
HENDERSONAnd, Kelley, I wonder if you could talk about how Juniper understands the journey she's been on so far.
FRENCHThere was a period of more than a year where she asked about her time in the NICU every single night. Tell me about when I was a baby, tell me about when I was born, tell me about when I was sick. And it got to the point where last summer I called the hospital and I said, hey, can I bring her to the NICU and just show her. And they were fantastic about it. And they let her come. And they set up an incubator in an empty room.
FRENCHAnd they let her play it in the room and she brought her little doll who was the size she was when she was born. The doctors and nurses who had taken care of her came by and listened to her heart. And Juniper played in that room for two hours. And she actually got to meet a baby who was less than a week old, who was born at 23 weeks. And that experience really answered her questions I think. And now she just waves it off. I was born very small and everybody was so worried.
HENDERSONThank you so much. Kelley and Thomas French. The book is "Juniper: The Girl Who Was Born Too Soon." Our best to you and to Juniper. I'm Nia-Malika Henderson…
FRENCHThank you Nia-Malika.
HENDERSON…with CNN, sitting in for Diane Rehm. Thanks so much for listening.
After 52 years at WAMU, Diane Rehm says goodbye.
Diane takes the mic one last time at WAMU. She talks to Susan Page of USA Today about Trump’s first hundred days – and what they say about the next hundred.
Maryland Congressman Jamie Raskin was first elected to the House in 2016, just as Donald Trump ascended to the presidency for the first time. Since then, few Democrats have worked as…
Can the courts act as a check on the Trump administration’s power? CNN chief Supreme Court analyst Joan Biskupic on how the clash over deportations is testing the judiciary.