Diane’s farewell message
After 52 years at WAMU, Diane Rehm says goodbye.
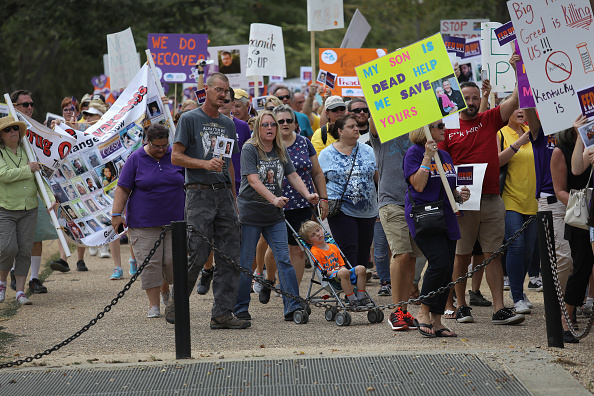
Activists and family members of loved ones who died in the opioid/heroin epidemic march in a "Fed Up!" rally on the National Mall on September 18, 2016 in Washington, DC.
According to the CDC, opioid-related deaths surpassed 30,000 last year for the first time in history. Diane and a panel of guests discuss why the numbers continue to rise, and what public health officials, doctors and advocates say needs to happen to reverse this alarming trend.
MS. DIANE REHMThanks for joining us. I'm Diane Rehm. According to the CDC, opioid related deaths surpassed 30,000 last year for the first time in history. Here with me to talk about what's behind this alarming trend and what can be done about it, Dr. Leana Wen, the Baltimore City Health Commissioner and Lenny Bernstein of The Washington Post. With us from Atlanta, Georgia, Dr. Thomas Frieden, director of the Centers for Disease Control and Prevention and from WSHU in Fairfield, Connecticut, Gary Mendell with the advocacy group, Shatterproof.
MS. DIANE REHMI do invite you to be part of the program, give us a call 800-433-8850. Send us your email to drshow@wamu.org. Follow us on Facebook or send us a tweet. And thank you all for joining us.
DR. LEANA WENNice to see you.
MR. GARY MENDELLThanks for having us.
DR. THOMAS FRIEDENThank you, Diane.
MR. LENNY BERNSTEINGood to speak with you, Diane.
REHMDr. Frieden, I'll start with you. Opioid-related deaths are the highest they've ever been. Give us some of the statistics.
FRIEDENThe bottom line is that we're seeing a continuing worsening of the opioid epidemic. We've seen a big increase in heroin deaths, a big increase and even bigger increase in deaths from illicit opioids like Fentanyl, very small but continuing increase in prescription opiate increases. And actually a decrease in deaths from methadone. But the big picture, in 2015, more than 52,000 overdose deaths, at least 63 percent of them due to opioids. Since 1999, prescriptions for opioids have nearly quadrupled and overdose deaths have more than quadrupled.
FRIEDENIn fact, since 2000, more than 300,000 Americans have died from opioid related causes.
REHMNow, Dr. Frieden, I want to relate to you a very personal experience. I fell, oh, five, six years ago and broke my pelvis in three places. As soon as I was admitted to a hospital, I was offered Percocet and I said, no, thank you. I would prefer simply to take Tylenol. And I can so vividly remember the nurse saying to me, but you're in pain. Percocet will help. Well, I had read enough about Percocet and the other pain killing drugs to know that I did not want Percocet. And I was fine with Tylenol. So what I'm wondering is, are these drugs offered too frequently, too readily, too often within hospitals and by physicians?
FRIEDENAbsolutely. We fundamentally need to improve the way we care for patients with pain and improve the care of people living with addiction. For both of those things, we're not where we need to be. Take them one at a time. For pain, exactly as you say, for many patients in pain, Tylenol or Motrin or a combination of those two will be just fine. I, myself, have had some very severe disc herniations, which are excruciating, Such that I couldn't walk, couldn't stand and I used only Tylenol and Motrin, never took an opiate for it.
FRIEDENAnd, in fact, was able to, with physical therapy, get back to going to the gym regularly. As we did our review, which was needed for us to issue the guideline that we did this past year on how to manage chronic pain as effectively as possible, as we did that review, we found that not only is there no evidence that opiates will improve outcomes in patients with chronic pain, but there is some evidence, not proof but some evidence, that patients who get opiates actually feel more pain and do worse.
FRIEDENSo they're not only dangerous because they can cause addiction and death, but they, in the long run, aren't helping. Part of the problem, though, is that often we want a quick fix. We want a quick result. And, yes, they will relieve pain very rapidly in the short term, but if we look at what will be best in the long term, what patients will do best with in terms of being able to work, being able to walk, being able to live fully without risk of overdose, there are many other modalities which is very important that insurers pay for so that patients can receive that can address pain.
REHMLenny Bernstein.
FRIEDENAnd just effectively or even more effectively.
REHMAs a health reporter for The Washington Post, you recently did a survey on prescription opioids. Tell us what you found.
BERNSTEINWell, we wanted to see what long term opioid use looked like in the United States and we surveyed about 800 people, 650 of them were people who say they used the drugs themselves for at least two months. Another 160 or so lived with them. And it presented both sides of the issue. There are people out there who told us, in no uncertain terms, that without their opioids, they would not function. A gentleman who said he'd be in a wheelchair. He wouldn't be able to walk.
BERNSTEINThey're -- people say I couldn't go to work because of my gout. So it presented the side that shows the reason why people are taking opioids. Notwithstanding everything that Dr. Frieden just said about using alternatives, which, of course, should be done. On the other hand, we found that more than a third said they were addicted or physically dependent on those drugs and that's probably a lowball number because a lot of people don't want to admit that.
BERNSTEINAnd we found that people were not getting advice from their physicians about how to stop taking these drugs. They went home with them. They got advice about side effects. They got advice about what not to do in certain circumstances, but really not very much counseling on how to stop taking opioids.
REHMTell me the brand names of the kinds of opioids you're talking about.
BERNSTEINOxycontin, Percocet, Vicodin, those are brand names. You might've heard them -- generics, oxycodone or hydrocodone.
REHMAll right. And turning to you, Commissioner, when -- I gather you've experienced this firsthand as a physician.
WENI have a confession to make, which is that when I look back at my medical practice in the ER, I have overprescribed opioids to many patients. I didn't mean to. I just didn't learn about how addictive opioids are. What we learned about was pain is a vital sign, that our goal, as physicians, is to treat this person's pain, to take away their pain. And so we used what we knew, which is opioids. Physicians need to do -- need to learn a lot more about how to have alternative methods of treating pain.
REHMSo what you're saying is that these brand name opioids have been made so quickly, easily available for physicians to prescribe, that when a patient presents with pain, you say, take this.
WENThat's right. And yet, we, as physicians and healthcare providers, do not get training on how to identify someone who may be misusing opioids and even what to do once we see a patient who has a substance use disorder. So we could be getting patients addicted ourselves, but not treating them then accordingly.
REHMHave you seen a patient who has become addicted? And if so, what did you do then?
WENEvery day, in the ER, I see patients who come in seeking help for their addictions. So many of our patients first start by using prescription drugs and then switch to heroin and then watch their lives spiral out of control. They ask us for help. My patients come in saying, I need treatment for my addiction. And I tell them, I'm sorry, but the wait for treatment is weeks or even months. The most recent Surgeon General report on this issue found that only one in ten people who need treatment for addiction are able to get it, which we would not find acceptable for any other disease.
WENImagine if I said, only one in ten patients with cancer could get treatment for it. So there are multiple problems, including that we have to change this pill for every pain culture. Not just by physicians, but also by patients, by consumers. And that we really have to treat addiction as the disease that it is.
REHMHave you ever seen a patient that you have prescribed an opioid, then switch to heroin and come back and ask you for help?
WENI have not, but that patient may be out there. I have seen patients who came in seeking help for addiction who I could not find treatment at the time that they need who then came in overdose and die. And I think about how we, in the medical system, failed that patient.
REHMDr. Leana Wen, she's the Baltimore City Health Commissioner and an emergency room physician. Short break here. Your calls, your comments when we come back. Stay with us.
REHMAnd as we talk about the rising number of individuals addicted to opiates in this country, many of whom have begun those addictions with prescriptions from physicians, I want to bring into the conversation Gary Mendell. He's founder and chairman and CEO of Shatterproof, that's an advocacy group dedicated to reducing addition. Gary, you started this group because your own son was addicted to opioids. Tell us about him.
MENDELLSure, sure. Well, my career was in business, and my older son Brian struggled with addiction to opiates for many years, and tragically on October 20, 2011, after having not used a substance for 13 months, he took his own life. So there's a double story, the one story of a young man who was addicted to opioids who did not receive evidence-based treatment, but there's also a story there of the shame and stigma that goes along with it, which was what was unbearable for him and caused him to take his life.
REHMHow did he get started on the opioids?
MENDELLHe -- he started as a typical teenager in America, where 13, 14, 15, 16, you start with beer or wine, and you move to marijuana, and then you move to opioids. And that's how it happened.
REHMAnd how did he get the opioids?
MENDELLVery easy to get in today's society. As Director Frieden said, we've gone from a society that was prescribing about 60 million prescriptions a year, 15 years ago, to about 230 to 240 million prescriptions a year today. And those prescriptions, instead of -- not only is it the number of prescriptions, which is four times what it was 15 years ago, it's the length of the prescriptions. They used to be for three or four or five days, and now they're 30 and 60 days.
MENDELLAnd so someone will take Vicodin, Percocet or Oxycontin for two or three days, and the other 27 pills will sit in their medicine cabinet, where that's where two-thirds of teenagers get it, in their parents' medicine cabinets.
REHMDr. Frieden, having heard all this in combination, it sounds as though physicians need more and better training in prescribing opioids.
FRIEDENThere's a lot that can be done to improve the care of both pain and addiction. As has been indicated, often opioids aren't necessary. When they are necessary, we encourage that the lowest dose for the shortest period of time is used. For patients on opioids, they need to be actively monitored for signs of addiction.
FRIEDENThere are also things that governments can do. State health departments can make sure that prescription drug monitoring programs are actively managed, used universally for all prescriptions, have the ability, ease of use, ease of interaction with electronic health records, allowing office staff to access, as well, so the doctor doesn't have to interrupt her or his work flow, making it easier for doctors to do the work there and actively managing them so that they identify which providers and which patients may need additional assistance.
FRIEDENWe have seen some states at least stop the increase in opiate deaths. We haven't seen big decreases, but if you look at places like Nevada and Florida, there they took it seriously, they improved policies, they've been able to at least blunt the increase. But we've currently really got two things that are driving this epidemic.
FRIEDENThe first is over-prescription of opiates, and I do want to make clear there are some circumstances for which they're absolutely necessary. We're not saying they should never be used. We're just saying they're very dangerous drugs, and patients and doctors should have an understanding of that, particularly for someone who's never had them. We don't want to create another generation of people who are addicted.
FRIEDENSecond we've seen a huge increase in illegal opiates, both heroin and illegally produced Fentanyl and other products. That's what has driven the really big increase over the last couple of years, particularly in some parts of the country, where the drug dealers are making these drugs and making them inexpensive and widely accessible. That's why it's so important that health, public health and law enforcement work together to identify where there are problems so that law enforcement can turn off the tap and stop this at the source so that these dangerous opiates become less available.
REHMHowever, Commissioner, when I'm questioning why use these drugs at all, if their usefulness can be short-lived, if there is such danger of becoming addicted, and if they become less effective in a shorter and shorter period of time, why prescribe them at all?
WENDr. Frieden said well that there are appropriate uses of opioid medications.
REHMSuch as?
WENSomebody comes in with a terrible car accident, they are screaming in pain, I can see their thigh bone sticking out. I mean, this is someone who needs opioids to take away their acute pain, someone who has cancer pain maybe towards the end of their life and needs management that other types of medications do not cover. But, and this is where the CDC guidelines under Dr. Frieden's direction really come into play, they say the aphorism of start low and go slow.
WENAnd that's what we should keep in mind, that we need to start with the lowest dose and go -- and advance slowly, look at other alternatives and know also that taking away pain is not our goal. If you call down and bruise you knee, pain may be okay. Just because you have pain doesn't mean that you need a pill to take it away. People need to -- all of us, not just doctors and big pharma, but we all need to switch our mentality so that it's not just this pill-for-every-pain culture.
WENAnd we have to ask one more question, which we have not yet, as much, which is what pain is it that we're treating. Is it just physical pain, or is there something deeper? When we look around, the areas that have had the highest rates of overdose and in substance use, these are areas with the highest rates of unemployment, unstable housing, uncertain futures.
WENThese are the same areas with higher rates of suicide, higher rates of overdose. Is there something beyond physical pain that we're treating?
REHMAnd Lenny, you found that in rural areas, for example, this has been hitting really hard.
BERNSTEINIt has. This is very bad in Appalachia. It's very bad in Southern Ohio. It's very bad in New Mexico. There -- for the first time in 20 years, the death rate for white woman in rural areas has gone up, and there was a landmark study that found this, and one of the main reasons is the abuse of opioids. There for the first time in 20-some-odd years, the life expectancy in America declined, according to the recent report that was put out by the CDC just a week or two ago. One of the main reasons was opioids, drug use.
BERNSTEINSo you can see it. You can plot it on a map, and you can see who is affected, and it is overwhelmingly people with less than a high school education, people of lower-middle-class income and people in rural America.
REHMSo as you look at what's happening in Baltimore, Commissioner Wen, how would you describe the situation there?
WENI would say that overdose is a public health emergency, which is what I declared last year. There are more people who die from overdose in our city than die from homicide, and it's not just the individual who's affected, it's also their family members, it's also the community. For so long in our city, addiction has been seen as a moral failing, and that's why when someone goes to jail, that's why when someone dies, it's seen as well, that's their fault.
WENWe're changing that mentality to focus first of all on saving lives. We got legislation changed so that as of October of last year, I became the single prescriber to every single one of our 620,000 residents in our city of the opioid antidote Narcan, and we've been able to save 531 lives just by everyday people, not medical professionals or even police, but just by regular people saving lives.
REHMDr. Frieden, I know you have to leave us now. Give us your last word on what you believe needs to be done to turn back this tidal wave, this epidemic of opioid use and death.
FRIEDENThere's no simple solution to this. It's going to require a series of efforts, including, as Dr. Wen said, all of us recognizing that pain is something that has to be managed, that there are times when it's absolutely essential to use opiates for it, but there are many times when there are much better, much safer ways to manage pain. Law enforcement needs to do more to reduce the flow of illegal drugs into our communities. State health departments can do more to provide doctors with the tools to more safely care for their patients. And all of us, finally, need to recognize that this is not something that's inevitable.
FRIEDENIt's extraordinarily unusual to see a cause of death increased like this in the United States. It's essentially unprecedented. And that's both a terrible thing, but also it tells us something. It tells us that this got worse because of human actions, and it can better because of human actions. We can turn this epidemic around. We can drastically reduce the number of people newly and unnecessarily exposed to opiates. We can improve care of those who are addicted, reduce the risk that those who are addicted will die and steadily reduce the numbers of deaths. But it's going to take all of us focusing, working hard and asking some hard questions.
REHMDr. Thomas Frieden is director of the U.S. Centers for Disease Control and Prevention. Thank you so much for joining us, sir. And now turning to you, Gary Mendell, tell us about Shatterproof and what you hope you can accomplish through that organization.
MENDELLSure. I think I absolutely agree with what Dr. Frieden said, that this -- there's no simple solution. But what I saw after my son's death was although there's no simple solution to the devastation caused by addiction and a subset of addiction, which relates to opioids, there are -- as a businessman coming in, there are simple things that can be done to dramatically reduce it. Ending it is complicated. Reducing it, I believe, is simple.
MENDELLFor example, let's take the opiate issue that we've been talking about here. There are five things that can be done. They all can be implemented within a period of months, not years, not one of them costs a penny, that can dramatically reduce this. Number one -- and it's all been referenced here, but they're simply, tailor it down to five things.
MENDELLNumber one, for those who are addicted today, they need treatment based on evidence. Over two-thirds of the treatment programs in this country, Commissioner Wen mentioned that only one in 10 of those addicted can access treatment, but the one in 10 who access treatment, only a third of them get treatment that's based on evidence. So you can get into treatment, but you're getting the wrong treatment. Can you imagine that for another disease?
MENDELLWe know what the evidence says. We're not requiring it. We should require it, number one, it doesn't cost a penny to do so. It can be legislated, or insurance companies can only reimburse evidence-based treatment, either one of the two will work. Number two, it's been referenced on this call, as well, Naloxone. Every one of the three million people who are addicted to opiates in this country should have access to Naloxone, paid for by insurance and readily available because just like anyone with a disease, a chronic disease, there will be relapse, and Naloxone needs to be there, can instantly reverse a life.
MENDELLNumber three, for those who are addicted to opiates, as well, and it's been mentioned on this call by Dr. Wen a few minutes ago, this is not bad people doing bad things. This is good people with a bad disease. The evidence is clear, brain scans show it. Let's treat people with this disease just the way we treat someone with another chronic disease, with roses not jail.
MENDELLNumber four -- the first three things I mentioned are related to those already addicted, but how do we prevent those -- the 300 million Americans who are yet to be addicted and future generations, our great-grandchildren and great-grandchildren to come. It's all been mentioned on this call, two things. No opiate should ever be prescribed again, starting tomorrow, unless a doctor has checked the prescription drug monitoring program.
MENDELLIt's simple, does not cost a penny. It can be delegated to a nurse, give the information to a doctor, and either doctors will start doing it voluntarily, or it should be legislated tomorrow. And the research shows that doctors who are not required to do it are only checking 14 percent of the time. Eighty-six percent of the time, they're not checking before they prescribe an opioid.
MENDELLNumber five, the CDC guidelines that were championed by Director Frieden, they came out in March. In a few months there will be a 10-hour continuing education course available to every doctor in the country for free. How long would it take every doctor in this country to take a 10-hour course that is online, they can take it when they want? If it were up to me, I would get every doctor in this country 60 days to take that 10-hour course, and if they haven't taken it at that point, their ability to prescribe opiates goes away until they do, five points.
REHMDr. Wen, talk about that CDC guideline, which does call for a 10-hour course. What's your thinking?
WENWe train medical students, nursing students, health professional students on many diseases, some of which only affect one in a million people. The surgeon general's report found that one in seven people, one in seven Americans, will face a substance use disorder in our lifetimes. It should be our responsibility to learn about how to prevent this disease, how to treat it, how to make sure that we ourselves are not complicit in it.
WENThis is, though, a broader cultural issue, and I want to also add onto what Mr. Mendell said in terms of things that can be done. There's one other, which is something that each of us can do today as patients, consumers and family members. We can ask the question. We can learn from you, Diane, and ask. During the break we were speaking that I look at all the patients that I've had, the number of patients who questioned whether they need opioids I can count on one, many two, hands.
WENAnd it should be a question to ask every time. Do I need this medication? What are the side effects?
REHMAnd we'll take a short break here. We've got lots of callers, lots of comments, which we'll get to when we come back.
REHMAnd welcome back. It's time to open the phones as we talk about opioid addiction, which has risen to critical numbers in this country. Let's first go to Bob in Rainbow City, Ala. Bob, I'm so sorry. You say you've lost your daughter.
BOBYes, I have. She died about a month ago. And we fought with her doctor. For years her doctor had been prescribing an anti-depressant pills. And then also opioids to sleep. And we finally -- she got addicted to them. She was abusing them. We let her doctor know it a long time. Finally got her off it. And then she had her first baby, 30 years old. And found out her doctor prescribed her right back on the same stuff. And she died.
BOBWell, I feel that society and the pharmaceutical society knew darn well what this stuff does. My doctor -- I had lower back surgery. And my doctor found out I was still on the opioids after 60 days 'cause my pain was getting worse. He told me 10 years ago, that can be causing your pain. He took me off it and my pain went away.
REHMThat's very interesting. And again, my sympathies for your loss. We did invite pharma on this program. No one got back to us on that. You know, this idea that so many people are on these drugs for so long, Lenny, and nobody's checking how long or what the reaction is.
BERNSTEINCorrect. I think one of the things that needs to be done is that people come in to see their doctor more frequently and that there be more testing when they do come in to see their doctor to see what's going on. Now, I understand the physicians' side of this. They are particularly primary care physicians, dramatically over-worked people who are already squeezing in many, many patients.
BERNSTEINAnd the idea that we would add another responsibility to their day and also the idea, according to some doctors, that we would be sort of telling them how to run their practice, is an ethi-ment to many, many physicians. And they feel like, you know, they're at the end of their rope already, spending hours after their workday doing paperwork. They're, they're terribly overworked. But something has to change. Can't, we can't keep going on like this.
REHMAnd of course, Gary Mendell mentioned among his five recommendations, Narcan. Talk about Narcan, Dr. Wen, and what it does and how it occurs.
WENNaloxone or Narcan is a complete antidote to opioids. This is remarkable because there are very few antidotes available in modern medicine. Imagine if I told you that you could get one medication that will save your life if you're dying from a stroke or a heart attack. I mean, we would -- this would be a miracle drug. In the ER I've used naloxone or Narcan thousands of times. And I've seen how someone who is -- who has stopped breathing and would otherwise be dead within minutes, will be walking and talking again, often within seconds of taking this medication.
REHMHow does it work? How does it work?
WENNarcan blocks the receptors in the brain that opioids would normally attach to. And so it completely blocks the effect of opioids and saves that person's life. That person literally will be walking and talking again.
REHMSo if an individual takes an overdose, if that individual has Narcan, it can stop one from dying.
WENYes. But only if somebody else has that Narcan. If you're overdosing yourself, you've stopped breathing. You're not conscious. You can't give yourself this medication. And that's why we in Baltimore have been getting Narcan into the hands of every single one of our residents. We believe this medication, at a time of a public health emergency, should be available in everyone's medicine cabinet, in everyone's first aid kit.
WENAnd that's why I wrote a prescription to every resident in the city. And we have done, since last year, over 17,000 trainings on street corners, in busses, in shelters, in public markets, because we believe that every bystander, family and friend should be able to save a life.
REHMAnd, Lenny, you say that many addicts themselves…
BERNSTEINYes.
REHM…now have Narcan.
BERNSTEINYes. In Baltimore in particular, in San Francisco, in some other cities they have been making Narcan available to drug addicts. It doesn't get anyone high. It's only use is to reverse an overdose. Well, unfortunately, the person who is more likely to be around when a drug user, a substance abuser has an overdose is another substance abuser. So why not put the Narcan in their hands, if you can?
REHMAnd what's your reaction to that Gary Mendell?
MENDELLI applaud wholeheartedly what Commissioner Wen is doing in Baltimore and agree with everything that both she and Lenny said. Another key part of it is, as Lenny just said, or -- and the Commissioner said, often when a person is not breathing, has dropped to the ground, there's someone else with them who has used a substance illegally. And so it's important to have Good Samaritan laws passed in states.
MENDELLShatterproof, in the last two and a half years, has been the lead advocate and then drafted legislation, brought on sponsors to the bills and got legislation passed in 11 different states related to, number one, Good Samaritan laws. Where if someone is with someone, they drop to the ground, they're not breathing, normally they would be afraid to make the phone call to an ambulance 'cause they might get arrested.
MENDELLBut if you pass a Good Samaritan law, the person making the phone call and the person lying on the ground cannot be arrested. So we've been very active getting that law passed in states. We've been also very active in states, getting laws passed to what Dr. -- Commissioner Wen said, which is getting it not only to the patient, but prescribing naloxone to people around them, third parties. And that needs legislation, 'cause doctors can normally just prescribe to a patient.
REHMAnd by the way, I misspoke earlier. Pharma did get back to us, but was unable to provide someone on the show. We have a tweet from Holly, who says, "A Los Angeles Times investigation detailed how drug companies are now pushing opioids intentionally with no recognition of risks." Lenny?
BERNSTEINWell, in 2007, Purdue Pharma pleaded guilty to misleading doctors, patients, regulators about the addictive qualities of Oxycontin, its long-lasting oxycodone. And so there is no doubt that at that time they were doing that. I've read these stories in the Los Angeles Times and the last one that came out a couple of days ago indicates that now that the sales of Oxycontin here in the United States are declining, that Purdue Pharma has adopted a strategy of beginning to market these in very similar ways all over the world. And that in other countries they may not be ready for this kind of marketing effort.
REHMHere's an email from Gary in Genesee, Idaho. "These deaths result from overdose, not dependence. Overdose is a mistake, not a weakness. Except for mistakes, these drugs are safe, even for those dependent on them. Please avoid blaming the mistake of overdose on drug dependence." Dr. Wen?
WENI agree with Gary, that we should be looking broadly. Not only at the problem of overdose, but also of addiction because we should think about addiction like other diseases. Let's say that somebody has a heart problem. They need to be saved at the time that they're having a heart attack. It's our job to save their life in that moment, which is what we do with Narcan or naloxone. Ultimately, we also have to get that person into long-term treatment. We would never hesitate if somebody has a heart problem to say they need that.
REHMHow quickly does one become addicted to one of these drugs?
WENIt depends on the person.
REHMTolerance.
WENIt depends on the person. It depends also on what else may be going on in their lives. Certainly, there are many individuals, as I think Gary is referencing, who really need opioids for the reasons that we mentioned earlier. And there are many other patients who've gotten -- many other people who've gotten addicted to opioids and other substances. It's our responsibility to provide treatment for these millions of people. This is the long-term treatment that we have to provide. And we really must change our mentality so that we're no longer incarcerating individuals who have the disease of addiction.
REHMLet's go to the Jeff in Lansing, Mich. You're on the air.
JEFFHi. Good morning, Diane. Thank you for taking my call.
REHMHi. Surely.
JEFFI grew up in northern rural Michigan. And several of my peers succumbed to opioid addiction. The lucky of us left the area and moved to more urban centers and haven't. And one of the things that, you know, I don't -- your panel has a lot of really wonderful ideas and they are working really hard. And everything that they've said is exactly true. But I fear that their efforts are collectively undermined by the elephant in the room that is wealth and equality and lack of opportunity.
JEFFBecause in my peers that I -- that did not leave the area, that stayed, it -- in my mind, from my perspective, they succumbed to the opioid addiction because they did not find a way to value their life without their addiction. And they could not find jobs or employment. They could not find opportunity. And, you know, there's a fundamental undermining that's occurring in our inner cities and in our rural areas that will continue unabated, that, despite all these good intentions, will not -- will save people, you know. But it's -- I'm really worried about the wealth and equality issue. And I know that that's not something your panel is situated to talk about, but…
REHMBut that's something you've written about, Lenny.
BERNSTEINYeah, I mean, you said it better than I can. There's no -- it's not a coincidence that the diseases of despair, drug addiction, alcoholism, suicide are occurring disproportionately in the places where jobs have left, manufacturing jobs have left, coal mines are being shut down. These are places where people are having a very difficult time finding jobs and supporting themselves. And, as I said earlier, you can see that it's disproportionately represented there. It's not an accident.
REHMDr. Wen?
WENWhen people can't see that tomorrow is going to better than today, that's when so many of our problems begin. And it's not just physical pain that people are treating, when it's all these other diseases, these problems of despair. And when they look out -- once they become addicted to these substances and then say, well, how am I going to get treatment, that aspect is lacking. We don't have nearly enough treatment, nearly enough funding. And that's what I hope all of us, no matter where we are in the country, will commit to.
REHMAnd you're listening to "The Diane Rehm Show." To Tulsa, Okla. Scott, you're on the air.
SCOTTHi, Diane. Thanks for taking my call.
REHMSurely.
SCOTTYou're gonna be missed.
REHMThank you.
SCOTTMy question is -- and to give you a little foundation. I am a criminal defense attorney in Tulsa. I have been for over a decade. And I lost my father in '08. And was prescribe Xanax. And Xanax turned into an opioid addiction and I've been clean for well over a year now. But my question goes further to possibly the amending or enacting of new criminal statutes in the states regarding maybe the pharmaceutical companies, but for sure the prescribing doctors and these pain management companies, that in my opinion, really are just licensed drug dealers.
SCOTTIn my work I deal with simples possessions, and possessions of intent on an individual level, but very rarely have I ever seen charges filed against doctors or anybody on the distribution side of it that are doing it, for lack of a better term, legally. And I'm just curious if maybe lobbying or something could help with that.
REHMLenny?
BERNSTEINThe DEA does file charges against doctors, pain clinics and other in the distribution side of it. There are a number of doctors in prison right now as a result of that. It's a slow process because you have a relationship with your doctor. It's a very private and sacred relationship. The only way that law enforcement can prove that abuse is occurring is by going into that office undercover, becoming a patient, and showing that the doctor really isn't doing anything except distributing drugs. It's a slow process.
WENI have worked with many hundreds, thousands of amazing physicians over the years. I don't know anyone, any of these doctors who knowingly would have prescribed someone too many paid medications. I mean, in retrospect, we now know that our practices were wrong. But it's a combination -- it's not -- yes, there are -- maybe the individual doctors who are running pill mills. And yes, they should be punished and held accountable to their actions. But the vast majority of the over prescribing is happening because of this culture of excess that all of us are complicit in.
WENAnd I want to say one more thing about doctors, too. It is extremely frustrating and disempowering as a physician when we see someone who has a substance use disorder, who we know needs treatment, but that treatment is not available. We need the tools to be able to identify patients at risk. To prevent addiction from happening, but also to be able to treat individuals at the time that they need it.
REHMHere's a caller that we don't have time to take, but Ashley is in Medford, N.Y., and says, "Please discuss where opioids might be the only solution." She says, "I have a rare neurological disease and opioids are very helpful." Dr. Wen?
WENIn one sentence, absolutely. There are some patients whom require opioids and we do not want for any guidelines to punish them. It's a question of being judicious about the use of opioids and just stopping this epidemic across the country.
REHMAnd do you plan to continue to write on this, Lenny?
BERNSTEINYes, absolutely. We'll be writing on it into next year.
REHMBecause?
BERNSTEINBecause the numbers are going up. They're not going down. And all the things that have been tried over the past 10, 15 years since we recognized the epidemic have not stemmed the overdose level. And we haven't even spoken about Fentanyl, which is -- has become the latest and most dangerous opioid in terms of overdoses. That -- the number of deaths from Fentanyl is going through the roof.
REHMWell, I'm sure there'll be much more talk on this. Thank you all so much. Lenny Bernstein of the Washington Post. Dr. Leana Wen, she's the Baltimore City Health Commissioner. And Gary Mendell, founder, chairman and CEO of Shatterproof. Thank you all so much. And thanks all for listening. I'm Diane Rehm.
After 52 years at WAMU, Diane Rehm says goodbye.
Diane takes the mic one last time at WAMU. She talks to Susan Page of USA Today about Trump’s first hundred days – and what they say about the next hundred.
Maryland Congressman Jamie Raskin was first elected to the House in 2016, just as Donald Trump ascended to the presidency for the first time. Since then, few Democrats have worked as…
Can the courts act as a check on the Trump administration’s power? CNN chief Supreme Court analyst Joan Biskupic on how the clash over deportations is testing the judiciary.