Diane’s farewell message
After 52 years at WAMU, Diane Rehm says goodbye.
Guest Host: Laura Knoy
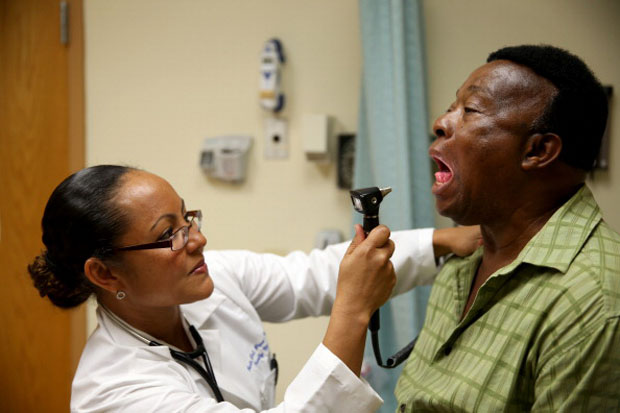
This 2014 file photo shows the newly-insured Felue Chang receiving a checkup from Dr. Peria Del Pino-White at the South Broward Community Health Services in Hollywood, Florida.
Health insurance companies have proposed rate hikes for individuals buying coverage on federal and state exchanges. In some cases, they’re asking to raise premiums by more than 40 percent next year. They say that too many people who signed up for coverage under the Affordable Care Act were in worse health than predicted – and that has cost insurers more than they had expected. But California and New York have managed to keep rate increases modest. President Barack Obama is urging other states to reject sharp increases as well. We talk about the economics and politics of insurance premiums – and what it all means for consumers.
MS. LAURA KNOYThanks for joining us. I'm Laura Knoy of New Hampshire Public Radio sitting in for Diane Rehm. She'll be back next week. Health insurers in some states are proposing to sharply raise rates on premiums. This will mostly affect individuals buying coverage on exchanges set up under the Affordable Care Act. Opponents of the ACA say rising rates are evidence of the program's flaws, but others say premium volatility is not all bad and more than 10 million American now have health insurance through ACA exchanges.
MS. LAURA KNOYJoining me in the studio to talk about the proposed rate hikes, Ron Pollack of Families USA and Douglas Holtz-Eakin of The American Action Forum. And from an NPR studio in New York, Susan Dentzer of the Robert Wood Johnson Foundation. Welcome to all of you. Thanks for being here.
MR. RON POLLACKThanks for inviting us.
MR. DOUGLAS HOLTZ-EAKINThanks for having us.
MS. SUSAN DENTZERGreat to be with you, Laura.
KNOYWell, Susan, I wanted to start with you. Just step back, please. Remind us of what these insurance exchanges are and who they're for.
DENTZERThe insurance exchanges were created under the Affordable Care Act. The big one, of course, is healthcare.gov. That's the national exchange run by the Department of Health and Human Services. And then, there are a number of state-based exchanges as well. Those exchanges have in them, available for eligible consumers, qualified health plans. These are health insurance plans that meet the criteria of the law and those are available for people who do not have another source of coverage.
DENTZERThe -- we're not about to go into the third year of open enrollment under the Affordable Care Act, which is why insurers under the law are now required to signal ahead of time if they intend to raise rates by more than 10 percent. So what we're hearing now is that share of plans that do intend to raise the rates that much. We're also starting, though, to get evidence that there are many, many other health insurers who are not going to raise rates that much for various reasons.
KNOYSo even though those double-digit increases, Susan, make headlines, it's more complicated picture than that.
DENTZERIt's very much more a mixed picture. We have some evidence that there are health insurers that are cutting their rates. For example, a recent analysis by the Kaiser Family Foundation showed you have a 10.1 percent decrease in plans in Seattle, Washington, on average, being proposed for 2016, versus a 16 percent increase in Portland, Oregon, just the state next door. So this is very much reflective of the differences in health insurance markets around the country, not to mention the very different ways health insurers have approached pricing decisions under the law.
KNOYWell, okay. So these are not for people with private employer sponsored insurance and they're not for people who receive Medicare or Medicaid benefits. These are for people, Susan, right, who sort of fall into that middle zone.
DENTZERThis was intended to reach out, largely, to those people who, as I say, had no other source of health insurance coverage, as you say, through an employer or other mechanism. So a number of people who were uninsured now, obviously, have access to qualified health plans under the law. Also, people who might be moving in and out of, say, employer-provided or companies, let's say, where they had access to coverage.
DENTZERSo, for example, now, we had in the past the experience where people stayed in jobs for long periods of time because they had health insurance through their employers. Now, they have the freedom to move out of those situations and potentially even set up their own business because they have access to health insurance through the exchanges, either at the state level or at the federal level.
DENTZERSo Ron Pollack, roughly, how many people are we talking about that fit that category Susan described?
POLLACKWell, there are about 10 million people who are getting coverage right now though the exchanges. I want to emphasize one point that Susan made and add two others. One of the points she made, which is very significant, is that the premium increases that are being proposed by insurance companies, the ones that have been publicized, they only need to publicize at this juncture those that have increases proposed in excess of 10 percent.
POLLACKSo a lot of the information about plans that are decreasing premiums or more likely increasing premiums, but at a much more moderate rate, we don't have the full picture. That's number one. Number two, when an insurance company decides that it wants to propose a significant premium increase, that's not the final word. Insurance agencies in each of the states reviews those proposed increases and what you see is, in state after state, the amount that's requested by an insurer actually is less, in the final analysis, than what was initially proposed.
POLLACKAnd the third thing, I think, that's very important to understand, one of the things we learned from this King v. Burwell Supreme Court case a few weeks ago, is we found out how important it is that people are getting premium subsidies that make health coverage much more affordable. 85 percent of the people who are in these marketplaces are getting subsidies. And these subsidies are extraordinary. I have, you know, I'll give you some examples from a few states.
POLLACKIn Florida, the average premium, without the subsidy, is $376. After the subsidy, they're only paying $82. They're getting a $294 subsidy on average. In Virginia, it's $348 is the premium. After the subsidy, it's $89. So as people...
KNOYSo a big savings for people. So when we see these scary headlines about premiums jumping 40 percent or 30 percent, folks will still get the subsidies, Ron, so they may not feel that giant hit. That's what you're trying to say there.
POLLACKYes. But the most important point is that the increases that we're seeing are the outliers right now, those that are in excess of 10 percent. Those which are small increases or even decreases, those have not been made as public because you're required to actually make public those that are increase of more than 10 percent.
KNOYSure. But if companies do get some of these more startling hikes, let's say they are approved, taxpayers will have to pay bigger subsidies, right, Ron, because that's how it's set up.
POLLACKYeah, there's no question. I think all of us on this program would agree that we've got to do something about the overall costs of healthcare and that's a common agenda for conservatives and liberals, Democrats and Republicans. So that's an agenda for the future.
KNOYI want to remind everyone that you're listening to "The Diane Rehm Show," and you can join us with your comments, questions, concerns, 1-800-433-8850. Send email to drshow@wamu.org. Again, 1-800-433-8850. Find us on Facebook or Twitter. So Douglas Holtz-Eakin, a couple years in now with these healthcare exchanges. How do you think it's going, given the premium rate increase proposals that we're hearing about?
HOLTZ-EAKINWell, I want to emphasize something that both Susan and Ron said, which is there isn't a one-size-fits-all story here. I mean, it differs county by county, whether it's Seattle or Portland. We looked at 40-year-olds to make it a nice fair comparison, 40-year-olds and the policy that existed last year and this year so it's a pure apples to apples comparison. And in 38 percent of the counties, the requested increases are 10 percent or more. So in 62 percent, they're not, right?
HOLTZ-EAKINSo we've got this very big difference across the states. There are some states where everything went up. There are three where all of the plans asked for more than 10 percent increase and there are about 9 where there were not substantial increases. So, you know, the truth will be in the final rates. We don't know those yet. We know California came in at 4 percent. Those have been pretty much finalized. It'd be interesting to know why.
HOLTZ-EAKINNew York's come in at 7.1 percent. And in a world with, you know, under 2 percent inflation, 7.1 is a substantial increase. So I think this matters a lot for people who are, you know, now obligated under the law to have insurance. It's illegal to not have insurance so they have to go to these exchanges and they have to get an insurance policy and it certainly matters to the taxpayers, who, as you pointed out, are going to end up picking up the bill for these increasing costs.
KNOYWell, it was interesting to look at some of the reasons insurers gave for why they had to ask for these double-digit increases.
HOLTZ-EAKINI think there's a lot of this which is still just start-up problems. I mean, this has been a rocky start-up at best and insurers say to the -- all the time, you know, this turned out to be a much more expensive population than we thought, right? We asked for rates expecting that we would get a fairly healthy group. We didn't. We have a much sicker than we expected. They had bigger bills than we expected and so we're trying to get the rates at the right level and that's a learning experience.
HOLTZ-EAKINThe fact that, you know, the state insurance commissioners are scrubbing these rates all the time and are granting some of these fairly large increases tells you there's some truth to that. And, you know, maybe that will stabilize and hopefully soon.
KNOYSusan, can you jump in there, too? I have read that insurers expected to get a younger, healthier population on these exchanges than they did and that's driving some of the costs.
DENTZERWell, that's true to some degree, but it really kind of depends on the insurer, as we've said. Insurers made very, very different decisions. Their actuaries made different calculations about how many young people would enroll and some plans pretty much called it the way things have turned out. So I don't think it's fair to generalize it in that respect. But to come back to this primary point, the main reason premiums are going up is that the cost of healthcare is going up and continuing to go up.
DENTZERNow, it's been going up more slowly for the past several years than it has been historically, but almost nobody thought that that was going to prevail over the long term. And one particular new phenomenon that insurers have noticed is we have a whole new series of very high cost so-called specialty drugs to treat very serious conditions, rheumatoid arthritis and especially Hepatitis C. And the Hepatitis C drugs are exceedingly expensive, $80,000, $100,000 for a course of treatment.
DENTZERBecause so many people, an estimated 3 million in the country, have Hepatitis C, many of these were people who were uninsured before the law was enacted. Now, they're insured and these drugs represent cures so insurers pay for them. But the costs are very, very high and so, for example, Blue Cross/Blue Shield of Minnesota, which has asked for an average 50 percent...
KNOYWow.
DENTZER...rate increases, cited the high-cost specialty drugs as a particular phenomenon and that is also playing out nationally.
POLLACKSo one of the things I think that's really important is take a look at how it compares with what happened prior to the Affordable Care Act and that might be worth a quick examination.
KNOYAll right. We'll do that after a short break. You're listening to "The Diane Rehm Show." Coming up, more on proposed healthcare premium rate hikes. Stay with us.
KNOYWelcome back. I'm Laura Knoy of New Hampshire Public Radio, sitting in today for Diane Rehm. We're talking this hour about proposed health insurance rate hikes, steep increases possible in some states. Our guests for the hour, Ron Pollack, executive director of Families USA, Douglas Holtz-Eakin, president of the American Action Forum, and joining us from an NPR studio in New York, Susan Dentzer, senior policy adviser at The Robert Wood Johnson Foundation and an analyst on health issues for the PBS NewsHour. Again, you can join us at 1-800-433-8850, drshow@wamu.org. Find us on Facebook or Twitter.
KNOYAnd all of you, let's go to our listeners now, and Julie's in Orlando, Florida. Hi, Julie, you're on the Diane Rehm Show. Thanks for joining us.
JULIEThanks for taking my call.
KNOYSure.
JULIEMy quick question, which I would like to address, is how plans are raising their premiums without having announced it. For example, last year my husband had the silver plan at about $200 a month, our portion. You know, that does not include subsidy. This year, the same company increased not their silver plan but the second from the lowest, the bronze plan, to over $450 a month.
JULIESo we called a healthcare.gov counselor and asked can you please help us find a better plan. And he was a very, very nice gentleman who helped us and said I can't believe it, why are costs so high. And then I said this is because this is Florida. Can you please address the fact that certain states have very high premiums that are not necessarily announced beforehand?
KNOYWow, really interesting, and Julie, I'm sorry to hear about your situation. Go ahead, Ron Pollack.
POLLACKWell, it's very different from one state to the other, and it's very different from one plan to the other in the same state. You know, in Maryland, for example, CareFirst BlueCross BlueShield has asked for a 30 percent increase. Cigna, on the other hand, has sought a three percent decrease in premiums.
KNOYWow, how often do you hear someone say decrease in health insurance premium?
POLLACKWell, you know, if you take a look at the Kaiser Family Foundation, they looked at 10 states, the biggest cities in these 10 states, where they had actual data about all of the different plans. And you had in Detroit, in terms of the average cost of these silver plan, it's being reduced from $230 a month to $226 a month. In Portland, Oregon, it's being decreased so that -- I'm sorry, in Seattle, it's being decreased from $254 to $228. So the bottom line that I think Julie needs to understand is that you have to shop.
POLLACKAnd the lowest cost plan in a state in year one or year two may not be the lowest cost plan in year three. And so people should not just renew in the plan they were in in the previous years...
KNOYDon't automatically assume it's going to work for you.
POLLACKBut they should look at the market.
KNOYHere's a question, though, at shopping around, though, and I want to let you jump in, too, Doug, but shopping around sounds great, Ron, but if shopping around means switching to a new doctor every year or two, you know, I don't want to do that.
POLLACKWell, of course, one of the things you have to do is you have to take a look at what are the overall costs, what are the premiums, what are the deductibles, what are the co-pays. But you also have to take a look at what the network is. And that's why it's really important for people to be smart shoppers. Don't just say the plan I had last year, it worked out pretty well. It may well be that there are significant changes in that plan, and you better look at options.
KNOYAll right, Julie, good luck to you. Go ahead, Doug, jump in.
HOLTZ-EAKINWell, I think Julie's call brings up three important issues. Number one, health care costs differ across the country, and so premiums are going to be different across the country. And Florida is a high-cost place. Premiums are higher in Florida.
KNOYAnd why is that, by the way?
HOLTZ-EAKINOne of the enduring mysteries of health policy is the regional differences in health care costs.
KNOYYeah, and it's frustrating for people in those states.
HOLTZ-EAKINPractice patterns differ. There are some demographic differences.
KNOYSure.
HOLTZ-EAKINYou can trace it to different things, but that's sort of point number one. Point number two is, you know, as she said, you know, the premium isn't the whole story. Yes, there's the premium. There might be a subsidy, as well. There's also the co-pays and deductibles, and some of these are quite big. I mean, the average, you know, deductible for a silver plan, the sort of benchmark plan in the exchanges, was $5,000, and that's a big chunk of money for people to cover. And co-pays and deductibles, you can have out-of-pocket maximums that get up to $5,600. So that's a big issue.
HOLTZ-EAKINAnd then there's the issue of, you know, can I really shop. And the average county has three choices, and I think one of the things to be concerned about going forward is genuine choice on these exchanges, as opposed to the notion of choice.
KNOYRight.
HOLTZ-EAKINAnd three is not a large number.
KNOYSome small states, like New Hampshire where I'm from, the first year had one insurer. So not a lot of shopping going on there. Well, joining us now by phone from Sacramento, California, is Yolanda Richardson. She's chief deputy executive director for Covered California, which is the state's health exchange. And Yolanda, from what I understand in California, you are not seeing double-digit increases this year. What are you seeing in terms of health care premium increases?
MS. YOLANDA RICHARDSONActually, this year we're very excited that we recently announced that California would be experiencing a four percent average increase across the state this year, which is actually lower than our last year's increase.
KNOYSo you're making Julie, our caller from Florida, jealous, probably. She's seeing a lot of increases. How was California able to do this?
RICHARDSONWell, a number of ways, actually, Linda. We, first of all, California embraced the Affordable Care Act very early on, and that included embracing the Medicaid expansion, which brought in very robust enrollment not only to Covered California but our Medicaid program, as well, which decreased our overall uninsured population by 50 percent. So that helped. In addition, Covered California has a role as an active purchaser, and what that means is we're very selective about the health insurers that we do business with, and so it's not just about rates, it's also about quality and the value of services that are brought to the consumers, who work directly with Covered California.
RICHARDSONIn addition, as an active purchaser, we have the ability to show the actual insurers who work with us where their prices, so that they know if they're not competitive, they will lose membership, which is very powerful in terms of the voice with the insurers. We also have standard benefit designs here in California, which help the consumers have the power to make the selection. So the plans are actually competing on price and network, and the consumers can choose based on what works best for them here in California.
KNOYWell, and you guys are in, also, a unique position, right Yolanda, in that you're huge, lots of people, and probably a lot of plans to choose from and to compete with each other.
RICHARDSONThat's correct. Currently, we went into this negotiation period with 10 health plans. We recently announced we've added two more. So we will start the year off with 12 health plans. So we think that's good choice for our consumers and definitely good volume.
KNOYWell, and one last question for you. We were just talking, Yolanda, about how different prices are from state to state. We heard from a caller from Florida, also a big state, so probably a lot of plans there. Do you have any advice from your position for insurance departments in other states about how they might get a better handle on this, even if they don't have some of the advantages that you have?
RICHARDSONYeah, you know, one of the things that here in California we found is very helpful is definitely about shopping and using the tools to find the best opportunity and price for the individual. And that's anywhere. That happens here in California. Rates are local. It may vary for people in Southern California than in Northern California, and we really advise our consumers to use our tools, look at the services that they need for their particular, unique situation and look at the price accordingly and make that choice for them.
KNOYAll right, Yolanda, thank you very much for your time, we appreciate it.
RICHARDSONNo problem. Thank you.
KNOYThat's Yolanda Richardson, again chief deputy executive director for Covered California, which is California's health exchange. Today on the Diane Rehm Show, we're looking at proposed health insurance premium rate hikes under the exchanges set up by the Affordable Care Act. Let's hear from you, 800-433-8850, drshow@wamu.org is the email. You can find us on Facebook or Twitter. And all of you, let's go next to Charles in Charlotte, North Carolina. Hi Charles, you're on "The Diane Rehm Show." Thanks for being here.
CHARLESThank you so much. I'm on my cell phone, so hopefully I'll keep a good connection. Just a comment and some responses from the panel, I'm a health care provider with a background in public health. I work for the Department of Veteran Affairs. I like outside of Charlotte, North Carolina. You know, we have very large hospital systems, and one of the things that happened in North Carolina is when the insurance companies were going to the hospital systems to try to negotiate a lower rate, the hospital system simply said no.
CHARLESThe hospital systems are a large stakeholder. I think the insurance companies were only able to negotiate around a six to eight percent decrease. So I'm interested in hearing the panel's comments regarding the hospitals and trying to control costs through hospitals as a stakeholder.
KNOYInteresting. So yeah, so Charles, don't just point the finger at the insurance companies. Look at the providers, especially these large hospital systems that have basically bought up all the doctors' practices. That seems to be what you're saying.
CHARLESYes.
KNOYYeah, thanks for calling in. Susan, can you talk about that? He makes a good point.
DENTZERAbsolutely, and this really underscores that rates are not rising in a vacuum here. They're related to the cost of care, and if you have areas of the country where you have dominant hospital systems, you get exactly the dynamic the caller described. Yolanda Richardson just alluded to the fact that the Bay Area of California has much, much higher health care costs than, say, the Los Angeles area. And that's because there are dominant health systems there that are resisting lowering prices.
DENTZERSo this is very much a fact around the country. It's one that health insurers have pointed to as a problem, sort of an unintended consequence of the law, which is that as hospital systems seek to consolidate, they do get more -- have more negotiating power and are resisting, in some instances, lowering their prices.
KNOYSure, and if they say no, that whole area is out of luck. Go ahead, Doug.
HOLTZ-EAKINThis is one of the real design flaws of the Affordable Care Act. You know, as Susan said, you know, this is not happening in a vacuum. Ultimately it is the cost of health care, and controlling the rising costs of health care was one of the main objectives of any health care reform. When the ACA went at this, one of the things it decided to do was form these things called Accountable Care Organizations. And the idea was let's get all the providers, the nurses, the doctors, the medical device guys, the MRI guys, get the hospitals, we get them all together, get them to coordinate the care for a patient, maybe do better at preventive care. It's a really good idea, in a vacuum.
HOLTZ-EAKINThe way they did it was to put the hospitals in charge and say you will organize the ACOs. So they made -- they increased the power of the hospitals enormously. There was already a trend toward consolidating. They were buying up doctors' groups and buying up all the providers. The ACA put that on steroids, and it's a deep concern from the competitive nature of all these local health markets. If you don't get good competition, you're not going to get costs down.
KNOYAgain, you can join us at 1-800-433-8850. Send email to drshow@wamu.org. All of you, we talked earlier about the price of medicines and how that's also inflating these costs. Here's an email from Kevin in Albuquerque, New Mexico. He says Congress should let the FDA negotiate drug prices with big pharma. Can you comment, Ron Pollack, on that real quickly?
POLLACKWell, right now, they're -- the federal government has actually been crippled from negotiating prices, particularly in the Medicare program. When Medicare added Part D that provided prescription drugs, there's a prohibition that prevents Medicare from bargaining for lower prices. And as Susan was mentioning, as more and more of these specialty drugs come to market, and some of them, it's $1,000 a pill.
KNOYWow.
POLLACKThe pill for Hepatitis C costs about $84,000 a year, and now there's a huge pipeline of drugs that are likely to come to market, and they're going to be very costly. But one of the things I think we want to make sure we don't lose sight of, and that's something that Susan alluded to. Before the Affordable Care Act was enacted into law, we were experiencing outlandish cost increases.
KNOYSo prices were going up anyway.
POLLACKPrices were going up. Premiums were going up. You know, I was just taking a look at what happened with employer-sponsored insurance costs, which is the predominate way that people get health coverage. Between 2003 and 2013, before the Affordable Care Act was being implemented, premiums, those paid by employers and employees, rose by 73 percent. And the cost of living rose only a tiny fraction of that.
POLLACKAnd those premiums were consuming 23 percent of the median family income. So before the Affordable Care Act was adopted, we were experiencing these significant premiums. The ACA has moderated those premium increases.
KNOYI'm Laura Knoy, and you're listening to the Diane Rehm Show. If you'd like to join us, call 1-800-433-8850. Send an email to drshow@wamu.org. Doug, did you want to jump in there?
HOLTZ-EAKINI do. I want to...
KNOYThe prices were going up already anyway.
HOLTZ-EAKINI just want to drag the discussion back to reality. First, I was the CBO director when the Part D program was passed, and this issue of negotiating came up again and again and again. And as CBO director, I wrote letter after letter to Congress, saying giving the secretary of HHS the power to negotiate will not lower the cost of this program.
KNOYCongressional Budget Office, and this is back...
HOLTZ-EAKIN2003.
KNOYPresident Bush, right, passed Medicare Part D. It was a big, big deal.
HOLTZ-EAKINRight, the Part D program has lots of competition in it. Prescription drug plans have to compete to get seniors. They then can turn around, if they have -- if they've got a big chunk of seniors, you know, six million seniors, they can cut a good deal with the pharmaceutical manufacturers, and indeed it's worked well enough that costs came in 25 percent below what I as CBO director predicted would happen back in 2003. So competition works.
HOLTZ-EAKINThe same is true with this Hep C drug. It was very expensive when it was introduced. There's now three of them, and the costs have come down dramatically. The number one thing you want to do is make sure you get good competition and keep new entrants into the drug market. We spend 10 percent national health spending on drugs. We spent 10 percent in the 1960s. So despite the repeated scares over costs of HIV, cost of specialty drugs, it's never turned into the issue that people have been concerned about.
KNOYIt eventually shakes out.
HOLTZ-EAKINSo, you know, the numbers are the numbers. And the last point in this is I'm concerned about the future because CMS just put out its projections for how fast health care spending will grow, and their projections for the second half of the next decade are to return to the rates that were there before the Affordable Care Act. We're going to grow about two percent faster than our incomes are growing. So it doesn't look like the ACA has changed the basic trajectory, and that's the number one problem that remains to be dealt with.
KNOYSo people should stop focusing on these -- or not stop but focus less on these premiums and look at...
HOLTZ-EAKINPremiums are one part of the story.
KNOYLook at what's really driving them, the cost issue.
HOLTZ-EAKINYeah.
KNOYI did want to share an email with all of you. This person didn't give a name. Please discuss the increased level of care and service people are receiving through their health insurance as a result of the ACA. The plans may cost more, but, this person says, they're also getting much more, preventative care, no lifetime maximums, no denials for pre-existing conditions, an overall better product for the money. This person says part of the rise in cost is also that people have fought ACA and demonized it. They conclude by saying if it was fully embraced and promoted, more younger people would sign up and help lower costs.
KNOYAnd this gets to something, Susan, we talked about before. Again, it does seem like younger people aren't signing up, and it is costing the insurers more to cover older, sicker people.
DENTZERWell, it is true that on balance, the population of people who have signed up for the Affordable Care Act so far, and insurers will tell you this, are somewhat older, somewhat sicker and somewhat more female than the general health insurance population with private coverage. In fact, there's -- on healthcare.gov, there's been about a 10-percentage-point difference in the number of women who have signed up versus the share of men.
DENTZERSo -- and what this just underscores is that people really needed this coverage. There were lots of women with, say, rheumatoid arthritis. One insurer told me that the single largest group of people they've signed up for the so-called platinum plans are people with cancers. I mean, no kidding, if you can cancer, cancer is a chronic illness, as we know now. People can suffer from it for years. You want the best coverage possible. So you go for a platinum plan.
DENTZERAnd I think to the emailer's point, we do have lots of new things covered, things that are covered now for everybody, like preventive services and mental health care. So those are very valuable services now, mandatory in qualified health plans.
KNOYComing up, more of your calls and questions on health insurance rates. Stay with us.
KNOYWelcome back. I'm Laura Knoy sitting in for Diane Rehm. We're talking today about proposed rate hikes in health insurance premiums. Our guests are Douglas Holtz-Eakin, president of the American Action Form. He was chief economist and director of the Congressional Budget Office from 2003 to 2006. Joining us from New York City, Susan Dentzer, senior policy advisor at The Robert Wood Johnson Foundation, and an analyst on health issues for the PBS NewsHour. Also with us in the study, Ron Pollack, executive director of Families USA. You can joins us at 1-800-433-8850. Email us at drshow@wamu.org. Find us on Facebook or Twitter.
KNOYAnd all of you, before we go back to our listeners, Ron, I know you wanted to jump in on this big question, why more young Americans aren't signing up for coverage on these Exchanges?
POLLACKWell, the Affordable Care Act actually provides some real helpful benefits for young adults. And most significantly, as we were talking before about the subsidies that are provided, these subsidies are provided on a sliding scale, which means the lower your income, the greater the subsidy you receive. Now, if you think about young adults, young adults tend to be in entry-level jobs, or they may not have a job. And so as a result, they disproportionately receive the benefit of these subsidies. And the more young adults learn about this, they will understand it truly is a value proposition for them to buy insurance.
KNOYWhy don't they understand that?
POLLACKWell, there's a very substantial portion of the American public that's still not aware of the subsidies. And one of the most important things we've been trying to do in terms of public education is to make sure that people learn about the subsidies. And the King v. Burwell case I thought was a teaching experience...
KNOYThat was a recent U.S. Supreme Court case, yeah.
POLLACK...because those subsidies would've been taken away. There's one other point, though, that Doug made. Doug made an interesting point that prescription drugs that we can moderate prices by competition. Well, that's -- you know, that's from an abstract notion that's absolutely correct. However, for a lot of these new drugs that are coming to market, there is no competition. There is no alternative. Now, he mentioned three different drugs for hepatitis C, but a whole bunch of these new drugs, these specialty drugs that are coming to market, there won't be any competition. And the pharmaceutical company can charge the sky is the limit. And there is currently no control that moderate those prices. That's something that needs to change.
KNOYOkay. Go ahead, Doug. And then we'll go back to our listeners.
HOLTZ-EAKINWell, on the young invincibles, one of the things that the Affordable Care Act did was this essential benefits, and it actually basically comes up with qualified health plans. Many of them had much cheaper insurance policies before the advent of the ACA. We saw triple digit increases in what young invincibles had to pay for a basic plan because of the ACA. And I think that harmed the effort to sort of get them to sign up. I mean, they had something they liked. It got taken away. It's now much more expensive, subsidies notwithstanding. And so, you know, their unwillingness to play ball with this I think is understandable.
HOLTZ-EAKINIt also I think raises just one of the fundamental divides about the ACA, in regards to where you come down, it's this issue of choice. The ACA says this is the essential health benefits, no choice, right? You get everything.
KNOYEvery plan must cover ABCDEFG.
HOLTZ-EAKINYou got to have these things. You know, I have to have maternity care on my insurance. That's the way it works. And then you have to buy insurance. It's now a violation of the law to not buy insurance. And which insurance do you buy? Well, in some places like California, there's an active purchaser. They're quite proud of that. But they're basically saying we're not going to let them pick from any plan. We're going to let them pick from the plans we like. And that limits the choice that they have.
HOLTZ-EAKINAnd you have to decide whether you're comfortable with that or not. And there are many people out there, conservatives in particular, who have valued the freedom of choice, and where freedom of choice in the rest of our economy has served us enormously well. And they don't want to sign on to this steady restriction of the choices that they have.
KNOYWell, I've heard that critique.
DENTZERLaura, Laura...
KNOYYeah, go ahead, Susan.
DENTZERI was just going to say there's one other point to make about young adults and the Affordable Care Act though, which is that there are other provisions that have enabled many young adults to get coverage. For example, in New York State, the Medicaid Authorities will tell you a lot of the people who are now qualified for Medicaid because of their income levels are in fact young adults. These are people who are, as Ron said earlier, starting out earlier in their careers, they're not making much money. Guess what? Their incomes are low enough that they now qualify for Medicaid.
DENTZERAnd also, as we know, early in the implementation of the Affordable Care Act, young adults were enabled to stay on their parent's health coverage up to the age of 26. And that's benefited at least another three and a half million or so young adult Americans today, and has cumulatively benefited a bunch of people over the last several years until they've aged out at age 26.
KNOYNow, that's interesting, Susan. So one reason you're saying that more young adults haven't signed up for these Exchanges like insurers hope they would is that they're going to Medicaid in those states that expanded, right? (unintelligible)
DENTZERThey have other sources -- exactly right. They have other sources of coverage.
POLLACKYou know, if you take a look at what happened in New York, Doug was citing that there was an increase of 7.1 percent. If you look at what happened in New York, compare it to what it was prior to the Affordable Care Act, what the New York State officials will say are the premiums are now 50% on average what they were prior to the Affordable Care Act. So there's been really significant improvements in a variety of places. Not just California, but New York has experienced an extraordinary improvement from where it was before the Affordable Care Act was enacted.
KNOYWell, and I've got a bunch of emails from Florida, people calling in responding to our earlier caller, frustrated that health insurance is so expensive in Florida. But I do want to go to a caller in Lebanon, Ohio. Hi, Janelle. Go ahead. You're on "The Diane Rehm Show." Welcome.
JANELLEHi, thanks for taking my call. I feel I'm representative of a group of people that's kind of been left out. I'm in a bit of a black hole. I turned 50 this year. My employer does not offer health coverage. I make enough to sustain myself, but I do not qualify for Medicaid because apparently up here income is not the only evaluation. I do not qualify for subsidies through the Affordable Care Act because they sent me a letter stating I make too little money for subsidies. And get anything offered through the ACA, it forces me to make a choice between a roof over my head or medical insurance.
KNOYWow.
JANELLESo I'd like to know how that's going to be addressed so that people like me aren't stuck in this position without healthcare at all.
KNOYSo why couldn't you get a subsidy, Janelle, on the Exchanges?
JANELLEI received a letter that stated my income was too low to receive a subsidy.
KNOYBut...
POLLACKSo Ohio does have...
JANELLEI even wrote a letter to the White House and received a response stating, we understand...
POLLACKSo Ohio is one of the states that has expanded the Medicaid program.
KNOYYeah, that's what I was wondering about.
POLLACKAnd so she should be eligible for Medicaid. Now, if she lived in a state like Texas that has not expanded Medicaid, and she's got income below the poverty level, she'd be in this no coverage zone. But in Ohio if you have income below 138 percent of poverty, so you should be able to get Medicaid. Now, if you have income above that, then you will qualify for the subsidies. You should not be in a no coverage zone.
KNOYDoug, you want to jump in?
HOLTZ-EAKINNo, I think that's exactly right. This is quite mysterious.
KNOYYeah.
HOLTZ-EAKINHer income's clearly too low to qualify for Exchange subsidy, she should be in the Medicaid program, and the expansion's been done. So I'm quite confused.
KNOYWell, good luck to you, Janelle. And thank you for calling in. Here's an email from David. "I am the CFO of a small company in Nebraska. We have experienced for our employees double digit increases with our employee plan for the last four years since elements of the ACA have gone into effect." David says, "This compounded number for us is a 64 percent increase over the past four years. We are now strongly considering discontinuing our healthcare coverage for our employees. We can no longer afford it, and the proposed employer penalty will be cheaper."
KNOYDavid concludes by saying, "The employees, including myself, will either forego coverage or purchase even more plans on the Exchange. Susan Dentzer, have you heard stories like this before? It's too expensive for firms to do this, so they just tell everybody to go on the Exchanges.
DENTZERAbsolutely. There is no question that that is happening in many areas of the country now. And, again, what element of this is related to the Affordable Care Act is a subject of some considerable discussion and debate. There's no question that in many instances plans now have to be better health insurance plans than they used to be. They've got the essential health benefits, as Doug said. They have to cover a number of preventive services. So the coverage, and of course as was also said, there are no more annual or lifetime limits. So the coverage is better on balance than it was before the Affordable Care Act, but it's also in many instances more expensive.
DENTZERAnd for small groups, in particular, small business, they face this very real consideration now. Is it better to basically give people some money to go and purchase coverage on the Exchange, or continue to run -- to essentially buy coverage on behalf of your employees? There's no question that that's an issue.
KNOYAnd I guess part of that calculation, Susan, right, is what state you live in. I mean, in some places which we're hearing the increases in premiums on the Exchanges isn't very much, and in other states it's a lot.
POLLACKAnd if you're in a small...
DENTZERAbsolutely, and it's also -- another thing that we haven't discussed is how many insurers are competing to sell insurance in particular states. And there still are states where there are dominant insurers and there isn't enough health insurance competition.
POLLACKAnd if you're in a small business, you're not required to provide insurance for your workers, if you've got fewer than 50 employees, so...
KNOYSound like David wants to though.
POLLACKSo -- yes.
KNOYSays he is now.
POLLACKYeah, yes. But I think we're going to see as small business owners determine whether they want to experience the same kind of high premiums that have risen well before the Affordable Care Act started and continue, they may take a look at what's happening in their individual market, and they may say to people, look, many of you are going to qualify for subsidies, for a family of four these subsidies are available up to $97,000 in annual income, and you may be doing a whole lot better. And so I think we are going to see folks going into the individual markets.
KNOYSo a shift away from employer sponsored care, more and more people going in the Exchanges, and that costs the government more money, right, Doug?
HOLTZ-EAKINYes. And I want to first take off my Congressional Budget Office hat and put on my small business owner hat. I started a think tank. I now have 30 employees. I am that person. I provide health insurance for my employees. And the ACA said that I had to buy my insurance through the equivalent of the individual Exchange called the SHOP Exchange...
KNOYThe SHOP Exchanges, yes.
HOLTZ-EAKIN...in Washington, D.C. And it constitutes one of the horrific experiences of my career. It does not work. And the notion that this somehow improves our ability to provide what we want to our employees is just hard to live with. I mean, it's expensive, it doesn't work, and it's the law that I have to use it. So that's a frustration from a business owner. And I've done the math.
POLLACKAnd the District is different in that respect than other jurisdictions, so let's be clear. What Doug was describing in the District of Columbia is not applicable in most states across the country.
KNOYAlthough I have heard frustration from small business owners...
HOLTZ-EAKINElsewhere, yeah.
KNOY...elsewhere over The Shop Exchanges.
HOLTZ-EAKINThe Shop Exchanges aren't working. It's an issue. But the fundamental point Ron was talking about is you can do the arithmetic, for anyone up to 300 percent of the federal poverty line, the employer can say, I'm done, stop providing insurance, pay the penalty, give the worker a raise out of the money that used to be health insurance costs. They can take their raise, pay taxes on it, go to the Exchanges and use the after tax income and the federal subsidies and get insurance that's better than what they had. So the arithmetic logic of getting out of the business of health insurance and sending people to the Exchanges is overwhelming. And the question is when will the employer start going that way?
KNOYSo are you going to go that way?
HOLTZ-EAKINI think about it. I really do.
KNOYAnd what's your hesitation?
HOLTZ-EAKINIt's the same hesitation that I think most small businesses have, which is there's an element of workplace culture and bonding that you want to have, so that you have the kind of cohesive organization that everyone desires. Changes of this type, you know, now we're going to give you the chance to disrupt all your provider networks. You have to go to a different doctor, get a different policy. It's not something you do lightly.
KNOYWell, I'm Laura Knoy, and you're listening to "The Diane Rehm Show." Again, you can join us on 1-800-433-8850. Send an email to drshow@wamu.org. Susan, I do have to ask you about this point that we've been talking about from the email, who says he's thinking about just sending his employees and himself to the Exchanges. This is a shift, isn't it, Susan, in the way health insurance has traditionally been provided? If more businesses make the choice that our emailer is making, then the government will be picking up more of the tab for health insurance, for everybody, right, if people get subsidies?
DENTZERYes. But, look, let's put this in a global perspective. We are the only large industrialized country that ties so much health coverage to employment. Almost no other country does it this way, because of all the reasons that have been described. And, you know, we ended up in this anomaly situation essentially for strange historical reasons. Health insurance was able to be given to employees during World War II without being subject to wage and price controls, the way wages were. So we stumbled into this big national experiment of tying health insurance coverage to employment. Now we're probably on our way stumbling out of it.
DENTZERBut, look, another very important point to make is that before the Affordable Care Act, small businesses in particular were dropping coverage in spades because it was so expensive. So this has been -- there's been a long-term trend of declining coverage in the small business community offering coverage to workers. And I think we're still on that trajectory, and it's going to continue to go down.
KNOYLet's take another call. This is Nino in Chapel Hill, N.C. Hi, Nino, go ahead. You're on "The Diane Rehm Show."
NINOHi, Laura. Great and necessary conversation. I would just like to point out that when I deal with any segment of our healthcare, I am not a consumer, I'm a patient. But I was calling because my premium went up last year 28.4 percent.
KNOYAnd you're on a federal -- on an Exchange, Nino?
NINOI'm on a federal Exchange because North Carolina tried to stay away from ACA as far as it can.
KNOYOkay.
NINOAnd so I sent the letter to the Blue Cross Blue Shield president and CEO. And wouldn't you know it, they called me within a week. And they explained to me that the reason why premiums went so high is that they grossly underestimated how many people are going to sign up through the Exchanges. They were expecting about 100,000 people and more than 250,000 people signed up. When I pointed out, well, doesn't that spread the risk, shouldn't that make it lower? He said that's disproportionately, those are people who are just young enough not to be on Medicare and people who had preexisting condition and didn't qualify for insurance before. And that number really outnumbered in a major way young people.
KNOYWow. So this is the story we've been hearing about, talking about all hour. Ron Pollack, go ahead.
POLLACKYeah, so I think the first people who signed up when the Affordable Care Acts that were open for business in 2014 tended to be, you would expected, those people who are most concerned about their health, people who've got chronic health conditions, people who are somewhat older, and so there's no question that at the beginning you had somewhat of a disproportionate percentage of the folks who signed up. They were somewhat older, they were somewhat sicker.
POLLACKI think as more and more people learn about the subsidies and they learn it's a good value because what they pay out of their own pocket is considerably less than they expected, I think you're going to see with each passing year, we're going to have a younger, healthier part of the population. And what that will do is it will put downward pressure with respect to the premium.
POLLACKSo it's not surprising that at the very beginning there's sort of a pent up demand, those people who are sick, those people who are old, I got to get coverage. And moreover, those people who are uninsured before who didn't get care before because they couldn't afford it, when they went and got insurance, they decided they needed to get sort of catch up with all the things that they hadn't gotten when they were uninsured. Those things are going to equalize as we look to the future. And I think that's going to create stability in terms of premiums.
KNOYWell, very quickly to you, Susan, all these insurers will be asking for rate hikes. State insurance commissioners don't have to say yes. What do you think, will they say yes to some of these big ones?
DENTZERThey already have said yes to some big ones, but we're going to see -- this is a big negotiating process and overall we're going to see rates come in lower than what the insurers have requested.
KNOYAll right. All of you, thank you so much for being here. I really appreciate it.
HOLTZ-EAKINThank you.
POLLACKThanks for inviting us.
KNOYI'm Laura Knoy sitting in for Diane Rehm. Thanks for listening.
After 52 years at WAMU, Diane Rehm says goodbye.
Diane takes the mic one last time at WAMU. She talks to Susan Page of USA Today about Trump’s first hundred days – and what they say about the next hundred.
Maryland Congressman Jamie Raskin was first elected to the House in 2016, just as Donald Trump ascended to the presidency for the first time. Since then, few Democrats have worked as…
Can the courts act as a check on the Trump administration’s power? CNN chief Supreme Court analyst Joan Biskupic on how the clash over deportations is testing the judiciary.